Colon pain can happen for many different reasons, and most of them are not serious. Common causes include things like gas, changes in digestion, or mild irritation. In some cases, it can be related to more significant conditions, which is why it’s important to pay attention to your symptoms. Here’s how to better understand what might be causing your discomfort, when to check in with a healthcare provider, and simple steps you can take at home to feel better.
My morning coffee is easily among my favorite parts of the day, but recently, my morning cup of joe has caused cramping pain in my lower stomach. Surprise: That’s where the colon is located. After a week or so of this persistent colon pain, I began to panic, wondering if it could be a sign of something serious.
After a bit of research and a conversation with a healthcare provider, I learned there are a lot of things that can cause colon pain, not just the serious conditions that first come to mind. In my case, rather than an underlying medical condition, it was more likely the stress of being in the middle of buying a home that caused my lower abdominal pain.
“For a lot of people, colon pain reflects how sensitive the gut is,” says Dr. Christina Le-Short, Medical Director and VP of Clinical Delivery at Override Health, a pain management specialist who regularly sees patients with abdominal pain. “Diet changes, stress, travel, and hormones can all affect digestion. It doesn’t always mean something structurally wrong is happening.”
Continue reading to learn about potential causes of colon pain, along with practical steps to identify the source and bring much-needed relief.

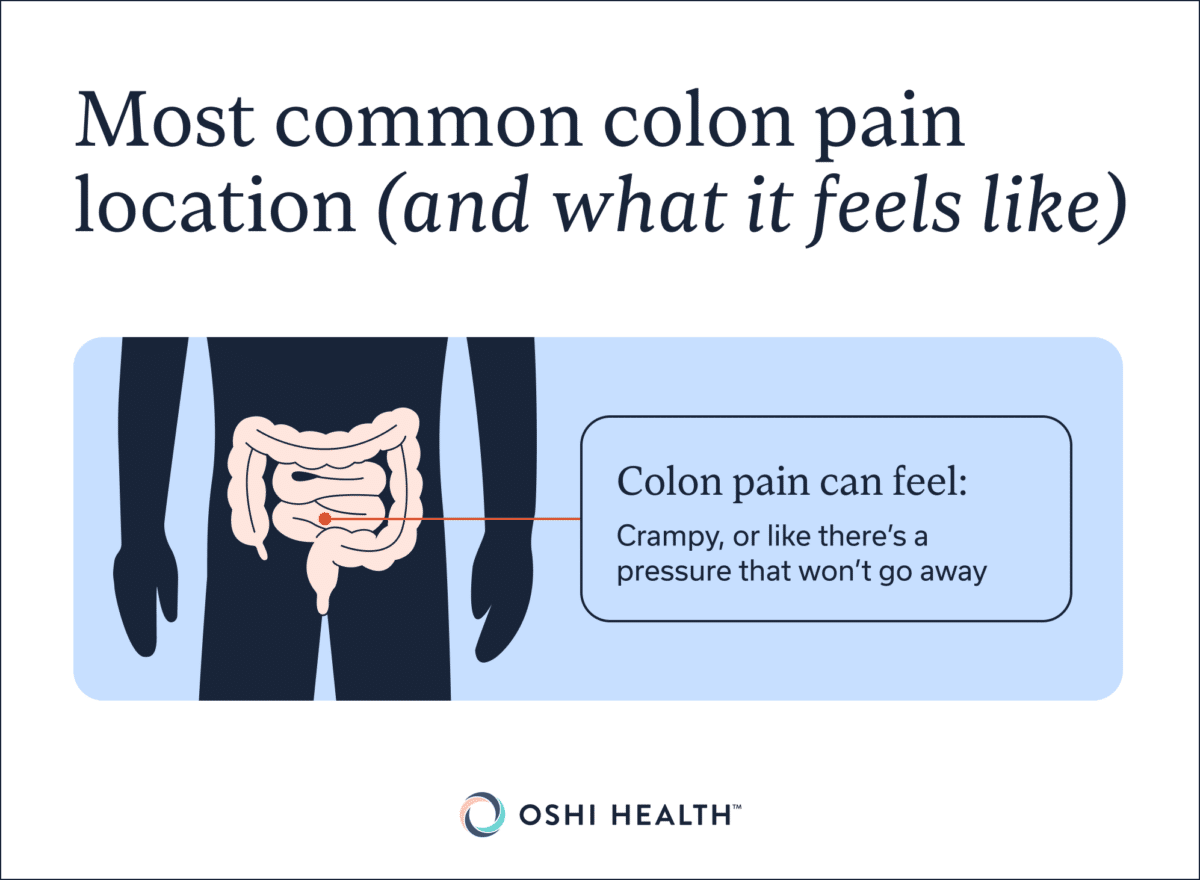
Colon pain location (and what it feels like)
The most common location for colon pain is the lower abdomen—and yes, that is a broad area. If you’ve ever looked at a graphic of the colon, you’ll know that it’s about five feet long, which is part of the reason why it’s hard to pin down an exact location for colon pain.
If you aren’t familiar with what the colon looks like, it’s a long, tube-like organ that connects the small intestine and anus. The colon is part of the large intestine, and food moves through it before leaving the body. The colon pulls out beneficial nutrients and electrolytes from food, and the rest becomes stool.
If someone is experiencing colon pain, what it feels like can vary depending on the cause and the individual. “When a patient is describing it to me, they will say things like’it feels crampy,’ or’there’s a pressure that won’t go away’ in their abdomen,” says Dr. Le-Short. She says patients also often report bloating, intermittent sharp pains, or that the pain comes in waves.
Because the ways people experience colon pain can vary so widely, it’s often difficult to pinpoint exactly where it is coming from. This is why you’re likely to be referred to a gastrointestinal (GI) specialist when you discuss your symptoms with a primary care provider or a pain management specialist.
Why does my colon hurt? The most common colon pain causes
If you’re experiencing pain in the colon, you may (understandably) be a bit panicked. Dr. Le-Short emphasizes that there are many potential causes, most of which are manageable and not as severe as colon cancer.
Constipation
Constipation is the sensation of needing to poop but not being able to. Most of us have probably experienced this at one point or another, and 12% of the US population has chronic constipation.
Too often, we dismiss constipation as just being difficulty pooping, but it can have far-reaching effects, including causing lower abdominal pain or pressure. “Constipation is a really common cause [of colon pain],” says Dr. Le-Short, “When stool sits in the colon too long, it stretches the bowel and creates that uncomfortable pressure.”
Diverticulitis
Diverticulosis is when small pouches form in the lower digestive tract, mainly along the colon wall. If those pouches become inflamed, it becomes diverticulitis (and yes, those two words are way too similar).
A main difference is that most cases of diverticulosis are asymptomatic, while diverticulitis usually comes with symptoms, which may include pain on the lower left side of the abdomen. Usually, this pain is severe and comes on suddenly. It’s usually accompanied by other symptoms too, such as a high fever, nausea, or vomiting.
Inflammatory bowel disease (IBD)
Another condition that may cause colon pain is inflammatory bowel disease (IBD), an umbrella term for chronic conditions that cause inflammation of the digestive tract. There are two common types of IBD: ulcerative colitis, which causes inflammation in the large intestine and rectum, and Crohn’s disease, which can cause inflammation anywhere in the digestive tract, from the mouth to the anus.
Along with lower abdominal pain, IBD usually comes with other symptoms too, such as weight loss, fatigue, nausea, rectal bleeding, and changes in bowel movements.
Irritable bowel syndrome (IBS)
Irritable bowel syndrome (IBS), a chronic gut health condition that leads to various abdominal symptoms, is another potential cause for lower abdominal pain. Dr. Le-Short says when IBS is to blame, patients often describe the pain as cramping. They also report other symptoms like bloating, constipation, or diarrhea.
If IBS is to blame, the pain may either improve or get worse after a bowel movement. Another tell-tale sign of IBS is when there are noticeable changes to how often bowel movements occur. Often, the stool looks different than usual, too, whether that means it’s more watery or harder than usual.
Sometimes, IBS is referred to as a” spastic colon,” since some people experience IBS pain as”spasms” (aka a sudden, involuntary cramp or twinge). This term, however, doesn’t accurately depict what IBS is or how varied its symptoms can be.
Trapped gas
If you find yourself asking, “Why does my colon hurt?” but there are no other symptoms and the pain isn’t chronic, the answer could be gas. “Sometimes it’s just truly just gas,” says Dr. Le-Short, “You’d be surprised at how sharp and intense gas pain can be.”
Most of us pass gas 13 to 21 times a day, either through the mouth, which is referred to as burping, or through the anus, which is referred to as farting. It comes from either swallowed air or the breakdown of digested food in the large intestine. If it gets trapped in the colon, it may cause pain on either the left or right side of the abdomen.
Occasional painful gas on its own usually isn’t a reason to see a GI provider. However, if it happens frequently or comes with other digestive symptoms, it’s a good idea to get it checked out.
Could it be colon cancer?
It’s hard to talk about the colon without the other”C” word (cancer) coming to mind. Colon cancer is serious, with a high mortality rate and a rising prevalence, especially among people under 50.
Colon cancer is not one of the most common colon pain causes, though lower abdominal pain is a common symptom of the cancer’s later stages. “Colon cancer usually causes pain when a tumor grows large enough to partially block the bowel or irritate the surrounding or nearby tissue,” explains Dr. Le-Short.
It’s important to note that pain is not common in the early stages of colon cancer. In fact, colon cancer’s early stages usually have few to no symptoms, which is part of the reason why colon cancer screening is so critical.
Another tricky thing with colon cancer is that the abdominal pain and other symptoms are nonspecific. This means they can overlap with conditions like IBS or IBD, and the only way to know for sure if symptoms are caused by colon cancer is to be screened by a GI provider, which usually involves a colonoscopy.
How clinicians evaluate colon pain
As a pain management specialist, Dr. Le-Short sees a fair number of patients who complain about lower abdominal pain. She often starts with a conversation around:
- What the pain feels like and any patterns (i.e., if there are triggers that make it worse or better)
- Any other symptoms they are experiencing, or any stool changes
- The patient’s lifestyle, diet, and stress levels
While the last bullet may seem unrelated, our gut constantly responds to the world around us. Just think of the last time you made a major life change, such as buying a new house or switching jobs. Odds are, your stomach was in knots at least once during the transition, which just goes to show how stressors in our lives really do impact gut health.
For undiagnosed abdominal pain, she typically refers the patient to a GI provider, who can complete a more thorough assessment and can order any appropriate testing, whether that’s a stool test, blood work, imaging, a colonoscopy, or a mix of tests.
After the assessment and once test results are in, a GI provider can make an official diagnosis and recommend treatment options. They may work with other healthcare providers, such as pain management specialists, registered dietitians, and gut-brain specialists, to manage symptoms and implement a treatment plan.
What you can do at home for mild colon pain
“There’s surprisingly a lot patients can do to help get some control back,” says Dr. Le-Short. She adds that meaningful improvement can come from even small changes, such as:
- Eating more fiber: Fiber is a type of carb that cleans out the digestive tract and keeps things moving. High-fiber foods, such as almonds, legumes, and quinoa, might help relieve pain when it’s due to digestive issues and also strengthen gut health overall for most people. But it’s nuanced; for some, increasing fiber intake could actually exacerbate symptoms, so it’s best to make any dietary changes under the supervision of a gastrointestinal (GI) provider.
- Staying hydrated: To stay regular, drink plenty of water throughout the day. When you’re hydrated, stool is often softer and easier to pass, which might help with mild lower abdominal pain.
- Getting in daily movement: Regular exercise may improve intestinal motility and reduce gut inflammation. However, if you are currently experiencing colon pain, opt for lighter exercise, like a walk or yoga class, over high-intensity workouts, such as running or CrossFit, which may exacerbate active symptoms.
- Paying attention to any triggers: Sometimes, things in our everyday lives trigger lower abdominal pain. Keeping a log of your symptoms in your phone’s notes app or a physical notebook anytime you experience pain, what you were feeling when it occurred, and what you recently ate, may help you identify triggers to avoid. Plus, this provides useful”gut health data” for a GI provider.
- Managing stress: “ When you’re anxious, overwhelmed, not sleeping well, or stressed out, your gut knows,” says Dr. Le-Short, “That’s why digestive symptoms often flare during stressful seasons of life.” While it’s impossible to get rid of all stress, there are strategies you can implement, like meditation, breathwork, or journaling, that can lower stress levels and help you become more resilient to stress.

When to see a healthcare provider
Colon pain doesn’t have to be debilitating to see a healthcare provider. Any pain that’s affecting your daily life is reason enough to make an appointment, whether that pain’s impact looks like constant anxiety over how close you are to a bathroom or canceling plans due to abdominal pain. “You don’t just have to live with a pain like this, especially when it’s interrupting your day-to-day,” says Dr. Le-Short.
Seek emergency medical care if the lower abdominal pain suddenly becomes so severe that it’s debilitating or if it’s present alongside:
- Blood in stool
- Vomiting
- A high fever
- Extreme diarrhea
Treatment options: How to”heal” colon pain by treating the cause
When we think of medical treatments, medications, and surgeries often come to mind. Depending on the colon pain cause, those may play a role in treatment, but addressing any GI conditions usually includes a more comprehensive, whole-person approach.
“Improving gut health isn’t just about medication or diet,” says Dr. Le-Short, “It’s the whole picture: sleep, stress management, movement, and paying attention to your body, mind, and emotions.”
That’s why working with a GI provider who understands that full context is so important. At Oshi Health, for example, patients work with a GI provider, such as a gastroenterologist, GI-focused nurse practitioner, or physician’s assistant, who can diagnose the underlying cause and create a treatment plan. They may then coordinate care with one of Oshi’s GI registered dietitians and an Oshi gut-brain specialist to make sure gut health is addressed from all angles.
Key takeaways
- Colon pain is usually located in the lower abdomen. Depending on the cause, it can feel crampy, like pressure on the abdomen, or sharp. This pain can be persistent, occur suddenly, or come and go in waves.
- Common causes of colon pain include IBS, IBD, constipation, and diverticulitis. When the pain isn’t accompanied by other symptoms or is ongoing, it could be due to passing gas.
- In rare cases, colon pain may be caused by colon cancer. That’s part of the reason why it’s important to see a GI provider if pain occurs–and why regular colon screenings are vital.
- Once a GI provider has determined what’s causing the pain, they’ll create a treatment plan. This may involve a mix of medications, dietary changes, lifestyle adjustments, and stress management techniques.
- Working with a GI provider who takes a whole-person approach, like Oshi, makes sure any pain and other GI symptoms are addressed from every angle.
Frequently asked questions (FAQs)
-
Pain in the colon can feel different for everyone. Some people describe it as a crampy, persistent pain, while others say it’s a sharp pain that comes and goes. It may also get worse or better after certain actions, such as going to the bathroom or eating.
-
A colon infection, referred to medically as colitis, has many possible symptoms. Common ones include lower abdominal pain, diarrhea that’s watery, blood in stool, and the feeling of needing to poop even when the bowels are empty. Depending on the type of infection, it may also cause symptoms outside the GI tract, such as a fever or fatigue.
-
Calming an inflamed colon often requires a multi-pronged approach. This may include a mix of medications, dietary adjustments, lifestyle changes, and working on the gut-brain connection to address any stress that’s contributing to inflammation.
-
If the colon is inflamed, the lower abdomen may hurt since this is where the colon is located. Many people report cramping or a persistent pressure when experiencing colon pain, though others describe it as a sharp pain or say it comes and goes in waves.
-
If colon pain interferes with everyday activities, consult a primary care provider or a GI specialist, such as the team at Oshi Health. When that pain is severe or gets suddenly worse, and is accompanied by symptoms such as a high fever, vomiting, or blood in stool, seek immediate medical care.
Oshi is your partner in digestive health
Feel like your digestive concerns are running your life? You’re not alone—and we’re here to help you find lasting relief.
Oshi Health GI providers, gut-brain specialists, and registered dietitians work together to address your symptoms and find solutions that actually work for you.
Whether you’re dealing with chronic digestive issues or unpredictable symptom flare-ups, our GI specialists deliver:
✔ Personalized care plans tailored to your lifestyle
✔ Science-backed strategies to calm your gut
✔ Compassionate, whole-person care
✔ And so much more!
Ready to take control of your gut health?