If you’re wondering “why is my poop bloody?” after your most recent trip to the toilet, you’re not alone. Up to 34 percent of people experience bloody poop at some point. Causes range from relatively minor ones that can be treated at home (like hemorrhoids), to serious emergencies (like colorectal cancer). It’s important to talk to a healthcare professional if you notice blood in your poop.
Seeing a streak of blood in your poop, or a red splotch on the toilet paper after you wipe, can feel scary. There are many possible causes of bloody poop, and some are more concerning than others.The color and amount of blood, along with your poop’s consistency, and any pain or other symptoms, can all provide clues to what’s causing your bloody stool.
Ultimately, some causes of blood in poop are minor, but many require urgent care and all merit evaluation from a medical professional. This guide will help you decide what to do next.
Why is my poop bloody? Common causes of blood in poop (most to least common)
Bleeding from your gastrointestinal (GI) tract is common, according to Kyle Eldredge, DO, a colorectal surgeon whose patients frequently see him after finding blood in their poop. Just because it’s common doesn’t mean it’s not serious, though.
“As a colorectal surgeon, I see this issue multiple times per day in my office,” he says. “While it may be embarrassing as a patient, this is often very treatable depending on the source, and [treatment] can greatly improve quality of life.”
Some potential causes of bloody poop, and their associated signs and symptoms, include:
| Cause | What it is | Signs and symptoms |
| Hemorrhoids |
|
|
| Anal fissure |
|
|
| Infection |
|
|
| Inflammatory bowel disease (IBD) |
|
|
| Anal fistula |
|
|
| Medication |
|
|
| Ulcers |
|
|
| Diverticular bleeding |
|
|
| Polyps |
|
|
| Colorectal cancer |
|
|
Keep in mind that while these are the most common causes of blood in your stool, there are even more causes than are possible to list here. That’s one reason it’s important to seek help from a GI care team, such as the GI providers who work with Oshi Health, if you find blood in your poop.
What does blood in stool look like? Common patterns and what they can suggest
The way that blood looks in your poop can actually signal where the bleeding is happening in your GI tract. Generally, GI bleeding is categorized as either upper or lower.
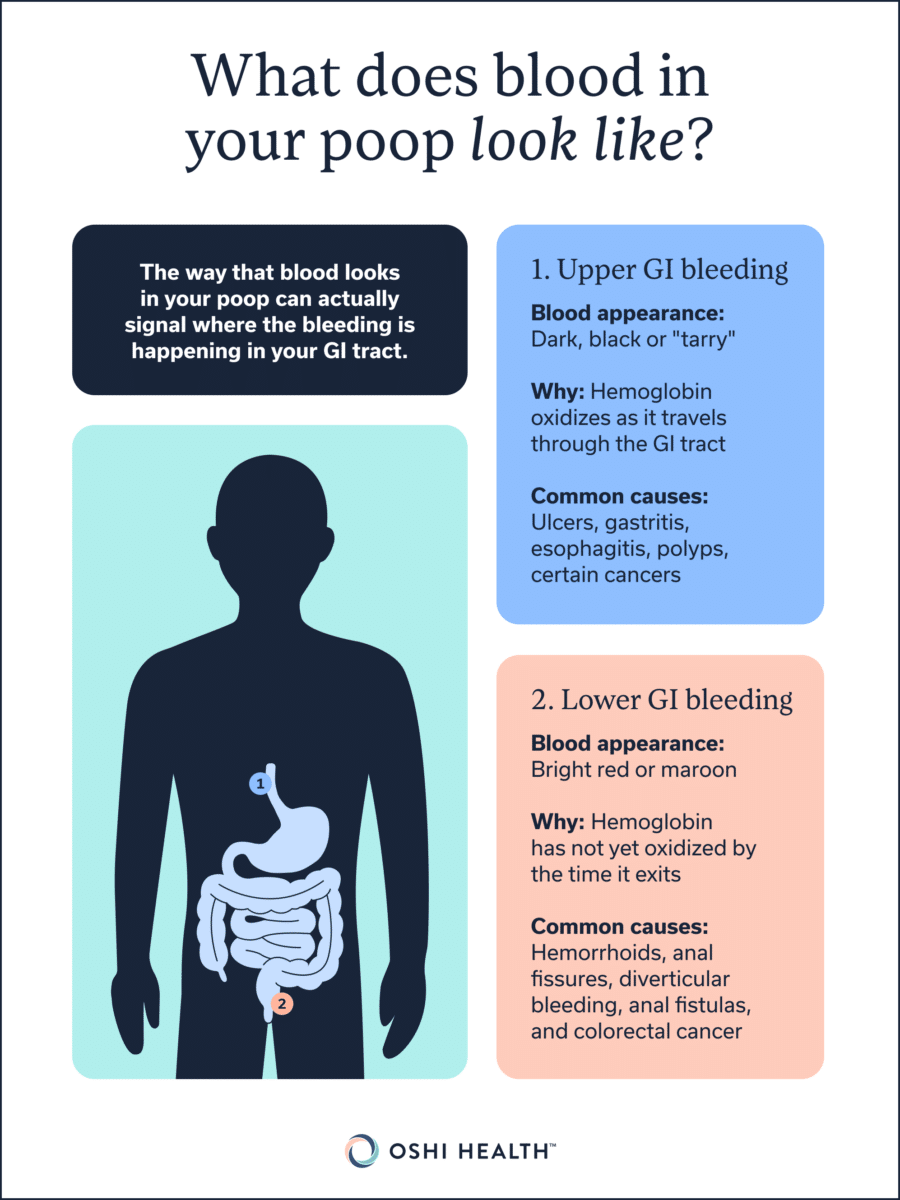
- Lower GI bleeding: Your lower GI system includes the colon, rectum, and anus. Lower GI bleeding is usually bright red or maroon in color, because the hemoglobin has not yet oxidized by the time it comes out in your poop. Examples of lower GI bleeding include hemorrhoids, anal fissures, diverticular bleeding, anal fistulas, and colorectal cancer.
- Upper GI bleeding: Your upper GI system includes the esophagus, stomach, and the first part of the small intestine. Upper GI bleeding is associated with dark, black, or tarry stools. According to Dr. Eldredge, this coloring is due to the oxidation of hemoglobin in the blood as it travels through the GI tract. Causes of upper GI bleeding can include ulcers, gastritis or esophagitis, polyps, or certain cancers.
There are also terms for the different appearances of blood in poop. These are:
- Hematochezia: A poop with bright red or maroon blood mixed in or streaked along it, or that leaves red blood in toilet paper after wiping. This is indicative of lower GI bleeding.
- Melena: A dark brown, black, or tarry poop that’s sometimes foul-smelling, and indicative of upper GI bleeding.
“Whether upper or lower GI bleeding, the bleeding may occur frequently and be noticed with every bowel movement, or may be very infrequent,” notes Dr. Eldredge.
In some cases, the bleeding is slow enough that you can’t see it with the naked eye. This is called occult bleeding and can be revealed by a stool test.
When it comes to the amount of blood in your poop, most times it’s a small amount either in the poop, on toilet paper, or possibly dripping into the toilet. Heavy bleeding with no pain could be a sign of diverticular bleeding, or something even more serious.
When blood in stool is an emergency vs when to call your doctor
So, you’ve found blood in your poop, and you’re feeling a bit anxious, concerned, confused, embarrassed, or all of the above. What’s next?
Shockingly, less than half of the people who experience rectal bleeding seek medical help. However, it’s very important to talk to a healthcare professional if you find blood in your poop—even if your hunch is that it’s something more common, like hemorrhoids.

“Any sign of bleeding should be evaluated by a medical professional,” confirms Dr. Eldredge. “GI bleeding can be due to cancer or precancerous polyps, and being evaluated can help save your life.”
Saying that, you don’t necessarily need to call 911 or rush out to the emergency room. You can use the severity of your symptoms to determine how urgent your situation is, AKA whether you should head to the emergency room, or if you’re good to make an appointment with a GI provider in the next week or so.
Go to the emergency room or urgent care
Some signs that you should seek emergency medical help include:
- A large amount of bright red blood
- Chest pain
- Lightheadedness or dizziness
- Severe pain accompanies the bleeding
- Shortness of breath
- Sudden bloody diarrhea
- Vomiting blood or “coffee grounds” substance
Make an appointment
“If occasional bleeding is noted with no other concerning symptoms, then talking to your doctor in their office may be appropriate,” says Dr. Eldredge.
If you’re looking to meet with a GI specialist from the get-go, consider booking with Oshi Health, where you’ll work with a full team of GI providers, registered dietitians, and gut-brain specialists with advanced training in GI conditions. As a virtual, multidisciplinary GI care clinic, Oshi can get you an appointment within days instead of weeks.
Diagnosis and testing: how clinicians evaluate bloody stool
Figuring out the cause of your bloody poop can take a bit of detective work. Your clinician will typically start by checking your health history. They may ask you questions about:
- Amount of blood
- Color of blood
- Consistency of your poop
- Family history
- How often you poop
- Location of blood (mixed in poop, on toilet paper, or in toilet bowl)
- Medications you take (especially NSAIDs, blood thinners, or antiplatelet medicines)
- Pain, swelling, or itchiness
- Recent travel or food eaten
Depending on the setting, your clinician may also perform a physical exam. This might include pressing on your abdomen, looking at your anus, or in some cases inserting a gloved finger into your rectum (to check for internal hemorrhoids).
It’s totally normal to feel nervous because, let’s face it, this exam doesn’t exactly sound pleasant. However, it’s very common and an important step in diagnosis. Be sure to let your clinician know if you’re feeling anxious, so they can reassure you. You can also always ask for a chaperone to be present.
Depending on the results of your health history and physical exam, your clinician might request additional tests. These include:
- Blood tests: A complete blood count (CBC) can reveal anemia, which is when you don’t have enough healthy red blood cells, and can indicate a GI bleed. Your blood may also be tested for inflammatory markers.
- Stool test: Your poop is sent to a lab to be tested for various infections, parasites, genetic changes that could indicate colorectal cancer, and more.
- Fecal occult blood test (FOBT): This stool test looks for blood in your poop that’s too tiny to see. It may be ordered if you have anemia, but no visible signs of bleeding.
- Colonoscopy or sigmoidoscopy: These procedures involve inserting a thin, flexible tube with a camera on its end from your rectum up into your sigmoid colon (sigmoidoscopy) or further up through your large intestine (colonoscopy). Don’t worry—you’ll be put under twilight anesthesia. These are used to diagnose polyps, diverticulitis, colorectal cancer, hemorrhoids, and more. Some treatments, such as removing polyps or potentially cancerous tumors, can also be done during the procedure.
- Upper endoscopy: If upper GI bleeding is suspected from black or tarry poops, then you might get an upper endoscopy. Similarly to a colonoscopy, this procedure uses a thin, flexible tube with a camera. However, the tube is inserted from your mouth, down your throat, and into your stomach and small intestine.
- CT scan: An abdominal CT scan can help find the location of a GI bleed, by using x-ray to create a 3-D image of your intestines.
- Nuclear medicine scan: Also called a gastrointestinal bleeding scan (GIBS), this imaging technique can identify active bleeds in your intestines.
All these questions, exams, and tests might sound like a lot, but it’s important to follow up with a GI clinician. Colorectal cancer is one of the most preventable cancers there is, according to Dr. Eldredge. Making an appointment with a GI clinician when you notice blood in your poop could potentially be life-saving.
Treatment options: what helps depends on the cause
The treatment for your bloody stool is, naturally, going to depend on what’s causing it. This can range from relatively straightforward lifestyle and diet changes, to new medications, to even surgery in some rarer cases.
Here’s a bit about what you can expect based on the most common causes:
- Hemhorrhoids: At-home remedies include drinking more water, eating more fiber (gradually), and taking a stool softener, to avoid straining. Your clinician might also recommend over-the-counter creams, ointments, or suppositories. More severe cases might require in-office or outpatient procedures.
- Anal fissures: First-line treatment typically includes fiber supplements, stool softeners, drinking plenty of water, and sitz baths. If symptoms persist, then you might try topical medications or botox injections. In the most chronic cases, a lateral internal sphincterotomy (LIS) procedure may be performed.
- Infection: For food poisoning and other infections, it’s best to rest, hydrate, and take prescribed medications (such as antibiotics or antiparasitic medication) depending on the cause of your infection.
- IBD-related bleeding: Your GI clinician will work with you on flare management to reduce inflammation, which may involve adjusting your meds.
- Anal fistula: Different types of surgery can treat perianal fistulas, depending on their severity and placement.
- Medication-related bleeding: Don’t stop any prescriptions on your own—your clinician will guide you through medication adjustments.
- Ulcers: Your GI clinician may prescribe medications, such as proton pump inhibitors (PPIs), H2 blockers, or antibiotics, depending on the cause and location of your ulcer. They may also recommend lifestyle changes, like adjusting your meds or quitting smoking. If an endoscopy is performed to diagnose an ulcer, it can also be treated at the same time.
- Diverticular or heavy bleeding: This might require urgent interventions or endoscopic treatment, which is done from inside your body during a colonoscopy.
- Polyps: These can be removed during the same colonoscopy when they’re diagnosed, with a procedure called polypectomy.
- Colorectal cancer: Treatment varies based on the stage of cancer, but can include surgery, chemotherapy, radiation therapy, immunotherapy, targeted therapy, and more.
Working with a healthcare provider: how to get answers faster
Consider booking an appointment with Oshi Health if you want to get to the bottom of what’s causing your bloody stool, but don’t have any emergency symptoms that require immediate care. Oshi’s GI clinicians can help you triage symptoms, discuss appropriate testing, and build a personalized treatment plan.
You can get the most out of your appointment by monitoring your symptoms and preparing at home. While you’re waiting for your appointment:
- Track details, including the color and amount of blood, frequency of bleeding, pain, stool consistency, and any triggers. Remember, nothing is TMI.
- Avoid straining when you poop. It can help to drink plenty of water, up your fiber gradually, and use stool softeners (if recommended by your clinician).
- Hold off on NSAIDs if possible. This class of pain relievers can raise your risk of GI bleeding. Be sure to ask a clinician about alternative pain relief options.
- Know your “stop monitoring” symptoms. Worsened bleeding, high-volume bleeding, dizziness, weakness, severe pain, sudden bloody diarrhea, and more can indicate an emergency.
The Takeaway
- Blood in poop has many possible causes—some minor, some urgent—but all warrant evaluation from a medical professional.
- The color and amount of blood, and any symptoms, can provide clues to what’s causing your bloody poop. However, it’s always recommended to see a healthcare provider if you see blood in your poop.
- Your healthcare provider will ask questions and run tests to identify the source of your bleeding, which will guide treatment.
- Head to the emergency room or urgent care if you experience large-volume bleeding, severe pain, dizziness, weakness, or vomiting.
Frequently Asked Questions (FAQs)
Is it serious if you poop blood?
Pooping blood can be due to relatively common causes like hemorrhoids or serious health conditions like cancer. You should take any blood in your poop seriously, and seek medical help.
How do you fix bloody poop?
There isn’t a simple “fix” for bloody poop. The first step is to get a correct diagnosis from a medical professional. Treatment depends on the cause, but can include anything from using stool softeners and eating more fiber to colorectal surgery.
Should I worry if there’s blood when I wipe?
It’s not uncommon to see blood when you wipe after pooping, but it’s still recommended to talk to a medical professional, because this can be a sign of some serious health conditions.
How much blood in your poo is worrying?
Any amount of blood in your poo is reason to see a healthcare provider, whether that’s a virtual appointment or an emergency room visit. If you’re experiencing heavy rectal bleeding, then head to urgent care or the emergency room. Otherwise, scheduling an appointment is acceptable.
Can food cause blood in stool?
Food doesn’t cause blood in stool unless there are other factors at play. For example, contaminated food can cause infectious colitis. Spicy or acidic foods could irritate pre-existing stomach ulcers. Both of these can lead to bloody poop. Some foods (like blackberries, beets, blueberries, black licorice, tomato skins, iron supplements, Pepto Bismol, or red food coloring) can also make your poop appear dark or red-streaked, but this isn’t from blood.
Oshi is your partner in digestive health
Feel like your digestive concerns are running your life? You’re not alone—and we’re here to help you find lasting relief.
Oshi Health GI providers, gut-brain specialists, and registered dietitians work together to address your symptoms and find solutions that actually work for you.
Whether you’re dealing with chronic digestive issues or unpredictable symptom flare-ups, our GI specialists deliver:
✔ Personalized care plans tailored to your lifestyle
✔ Science-backed strategies to calm your gut
✔ Compassionate, whole-person care
✔ And so much more!
Ready to take control of your gut health?