Gastroparesis is a chronic condition in which your stomach muscles have trouble moving food into the small intestine. This leads to a buildup of food in the stomach, which can cause uncomfortable symptoms. Fortunately, making small but meaningful dietary changes can help alleviate symptoms while helping you maintain optimal nutrition.
Your stomach is quite the workhorse. Its muscles act like a pump, mixing, churning, and moving food into the intestines. But under specific circumstances, the muscles and nerves can stop working as effectively.
Having gastroparesis, also called delayed gastric emptying, means your stomach muscles have trouble doing their job, leading to symptoms such as early fullness when eating, nausea, vomiting, and stomach pain.
Identifying the cause isn’t always straightforward. The stomach muscles might be impaired because of underlying conditions, nerve damage, surgery, medication side effects, and more. And sometimes the cause is idiopathic, meaning unknown.
Dietary changes can be helpful for gastroparesis, but you might be wondering why diet matters and how to harness it to help you feel better.
In this article, we explore gastroparesis causes, diets for gastroparesis, gastroparesis self-care , and more.
Gastroparesis basics: The condition and its causes
Gastroparesis is a condition that causes symptoms of abdominal pain, nausea, vomiting, fatigue, and feeling full early while eating. These symptoms can lead to malnutrition, rapid weight loss, electrolyte disturbances, and other complications (like bezoars or Mallory-Weiss tears).
Management of gastroparesis through diet and other strategies helps alleviate symptoms and reduces the risk for complications. Understanding the condition and what causes it can be helpful in deciding on next steps. That said, figuring out the reason isn’t always a straightforward process; about half of cases are idiopathic, meaning they have no identifiable cause.
Other causes damage the vagus nerve (which controls stomach muscles), other nerves, or stomach muscles or anatomy.
Gastroparesis causes:
-
Autoimmune conditions or endocrine abnormalities, such as underlying thyroid and diabetes
-
Diabetes
-
Idiopathic (cause unknown)–most common
-
Neurological conditions
-
Medications
-
Rheumatological diseases
-
Surgery
-
Traumatic spinal cord injury
-
Viral infection or post-infectious gastroparesis
As noted, medications can cause gastroparesis as a side effect. These include, but are not limited to:
-
Antidepressants (tricyclic)
-
Dopamine agonists
-
Calcium channel blockers
-
Mood stabilizers
-
Opioids
-
Progesterone (hormone therapy)
Diet for gastroparesis: The core principles that help most people
If you have gastroparesis, working with a GI registered dietitian can be helpful. They can ensure you’re getting the right nutrition for you, are able to eat as many of the foods you enjoy (including those important to your culture), and can still properly manage any co-occurring conditions, such as diabetes.
You might be searching for the right foods for gastroparesis. So let’s explore some gastroparesis diet modifications. Not one specific diet or set of foods is recommended for the condition. However, these general strategies tend to help people manage their symptoms while still getting enjoyment out of eating.
One thing to keep in mind: If you are experiencing a complication right now, you should talk to your doctor about which dietary strategies are right for you. In some cases, you may need to temporarily be on a liquid or bland diet until the complication resolves or you may need additional treatment.

Eat small, frequent meals
Gastroparesis can make you feel full fast, even after just getting started on your meal. This can hinder your ability to take in enough nutrients to maintain your weight and get all your necessary macronutrients (protein, fats, and carbohydrates) and micronutrients (vitamins and minerals). Additionally, feeling full can lead to abdominal discomfort.
For these reasons, you may need to stray from eating just three main meals a day. Eating smaller and more frequent meals might be a better solution. For example, in addition to a small breakfast, lunch, and dinner, you might add a mid-morning, late-afternoon, and post-dinner snack.
Stick to a lower-fiber diet
The health benefits of fiber are numerous, but if you have gastroparesis, you may need to reduce your fiber intake a bit. Fiber slows gastric emptying, so it can worsen gastroparesis symptoms.
Healthy adults should aim for a fiber intake of 25 to 35 grams per day, with males aiming for the higher end of the range. But if you have gastroparesis, you might need to stick to just 10 to 15 grams of fiber per day. Sometimes, however, individuals with gastroparesis can tolerate more than that. A registered dietitian can help dial in targets that are right for you and modify the texture and particle size of fiber foods to improve your tolerance.
Additionally, the fiber type you choose also matters. You may wish to stick to soluble fiber options, rather than insoluble, as much as possible. Soluble fiber forms a gel-like substance when it dissolves in water, whereas insoluble fiber passes through the GI tract largely undigested if not chewed adequately, which can up your discomfort with gastroparesis.
Many people find that cooking fruits and vegetables is also a great strategy to aid digestion processes.
Eat a lower fat diet
Fat is a necessary component of any diet. However, fat slows digestion, which could leave you with worsened symptoms or feeling fuller even faster and lacking an appetite for longer.
For this reason, spreading your fat consumption throughout the day and generally having a lower intake can be beneficial.
Additionally, how you consume fat may matter. Some research shows that fat in a liquid format, as opposed to in a solid meal, may be better tolerated in people with gastroparesis. You should work with your dietitian to find healthy fat sources that you can still include in your diet in small portions–this is necessary for the absorption of fat-soluble vitamins.
Again, a registered dietitian can help you dial in the amount specific to your unique needs.
Keep texture in mind
In addition to following the above recommendations related to fiber and fat, you might find that the texture of food matters for symptom relief. Softer foods can generally be easier to digest. Think applesauce instead of apples.
Additional pureed options might also be beneficial. Baby food, fruit puree pouches, smoothies, meal replacement drinks or powders dissolved in a liquid, blended soups, oatmeal, and more can all help you up your nutrient intake without upping your discomfort.
Gastroparesis self-care
In addition to dietary changes, some self-care strategies can also help you manage your symptoms.
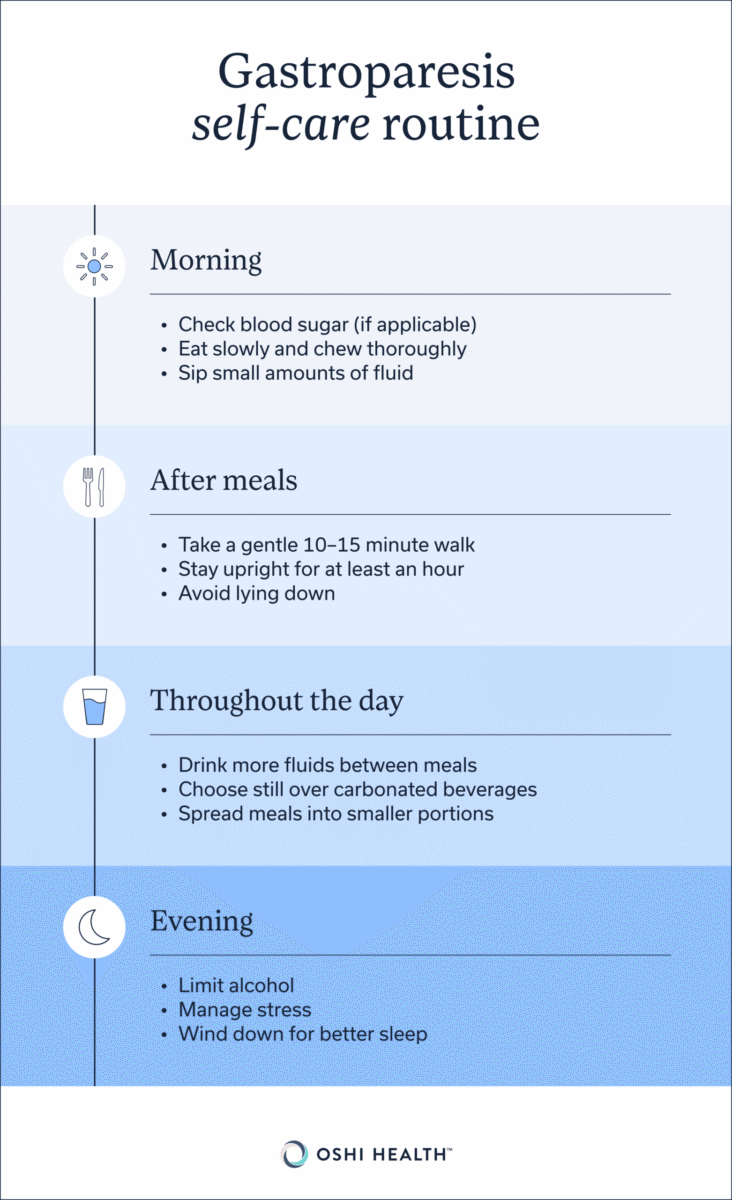

Manage blood sugar
Diabetes is the most common condition associated with gastroparesis. Over time, high blood sugar can damage nerve cells and impair how your stomach muscles contract. Additionally, certain medications used to treat type 2 diabetes can lead to delayed gastric emptying.
Maintaining good glucose (blood sugar) control is crucial for all forms of diabetes. And doing so can be helpful for reducing symptoms of gastroparesis.
Blood sugar spikes from high-carbohydrate meals increase GI tract sensitivity, which could worsen gastroparesis symptoms.
Complicating matters is that some of the dietary strategies for controlling high blood sugar, such as boosting fiber intake, can also worsen symptoms. Therefore, if you have gastroparesis and diabetes, working carefully with a registered dietitian can help you create a nutrition plan that takes both conditions into account.
Chew thoroughly
The more you can do to help your body digest food, the better. One simple tip to help alleviate gastroparesis symptoms is to chew each bite of food thoroughly before swallowing.
Move after meals
Movement after meals can perform double duty for gastroparesis. Research shows that gentle exercise, such as walking, after eating helps reduce fullness and bloating. Additionally, exercise after eating can help lower blood sugar.
Avoid lying down after eating
Stay upright after a meal for at least an hour, if not longer. Lying down can further delay gastric emptying and worsen symptoms.
Stay hydrated, but strategically time fluids
Hydration is crucial for everyone. With gastroparesis, you might not feel like drinking fluids sometimes, simply because of feeling full, but you still need to stay hydrated.
A possible strategy is to take small sips of water or another beverage during meals. Then up your fluid intake between meals. If you consume a lot of liquid during a meal, the fluids may make you feel fuller faster and limit the amount of nutrients you take in.
Minimize carbonation
Carbonated beverages, whether soda, sparkling water, or other fizzy drinks, can cause bloating, distention, and pain because of their carbon dioxide bubbles. Choosing still beverages as much as possible is likely best.
Limit or avoid alcohol and quit smoking
Alcohol consumption damages the GI tract, and it slows gastric emptying. Both issues can worsen gastroparesis symptoms. Plus, the liquid from alcoholic beverages can fill you up fast. If you have gastroparesis, limiting your alcohol consumption or abstaining altogether can be beneficial.
Likewise, the negative effects of smoking tobacco on health are well-known. What may not be as obvious is that smoking can delay gastric emptying. Smoking drives inflammatory processes in the body, which can also damage the nerves of the GI tract and worsen gastroparesis.
Limit ultra-processed foods
Ultra-processed foods contain added sugar, added sodium, preservatives, dyes, and more. These are all additives that can impair gut health and worsen symptoms.
That being said, sticking to a completely whole-foods diet can be challenging and unrealistic, especially with gastroparesis. So you may need to incorporate some processed foods that are easy to digest. Examples include meal replacement drinks or powders. A registered dietitian can help you choose options that make the most sense for maintaining optimal nutrition while avoiding harmful additives.
Support your mental health
Gastroparesis doesn’t just affect digestion; it can also affect your mental health. The condition is associated with mental health concerns such as anxiety, depression, and stress, and can certainly affect your quality of life. After all, having a full stomach or uncomfortable symptoms after eating can make you feel sluggish, low-energy, and impact how you feel in social situations involving food.
Mental health and GI health share a complex relationship, too: The brain and GI tract communicate via what’s called the gut-brain axis. This communication pathway can become impaired or disrupted and cause gastroparesis symptoms to worsen.
For these reasons, treating underlying mental health conditions and managing stress are an important part of managing gastroparesis. Additionally, working with a gut-brain specialist or psychologist can help you strengthen your gut-brain connection, which may alleviate gastroparesis symptoms.
Get adequate sleep
Getting good quality sleep supports overall health, including GI health and mental health. Aim for at least seven hours of sleep per night with minimal interruptions.
Keep a symptom log
You may find that keeping a log of your diet, stress levels, other mental health symptoms, and your gastroparesis symptoms is helpful. A log helps you or a clinician see patterns regarding what triggers your symptoms. Once you’re aware of specific triggers, you can take steps to reduce them and potentially reduce your symptom frequency or severity.
Working with an Oshi healthcare provider
As we’ve covered, gastroparesis and overall GI health are affected by many factors, so you may benefit from coordinated, multidisciplinary support from Oshi Health.
Your care team might include a GI provider (a nurse practitioner or physician associate), a GI registered dietitian, and/or a gut-brain specialist or psychologist, all overseen by board-certified gastroenterologists. They collaborate to help you improve your gut health, determine if you have underlying conditions, and, in the case that you do, help you manage them.
Key takeaways
-
Gastroparesis is a chronic condition that delays stomach emptying, leading to feelings of fullness, bloating, and discomfort.
-
Sustainable dietary changes, such as eating smaller, more frequent meals, may be beneficial.
-
Oshi Health can help you tailor your diet for optimal nutrition, symptom management, and food enjoyment.
FAQ
-
Rather than sticking to specific foods for gastroparesis, clinicians typically recommend overall dietary strategies (tailored to you) for managing the condition. These include eating smaller meals and eating more frequently, focusing on hydration between meals, reducing fiber and fat consumption, and sticking to softer and easily digestible foods.
-
Gastroparesis flares can be triggered by eating too much or too quickly, having high blood sugar, drinking too much liquid at meals, eating high-fiber or high-fat meals, drinking alcohol, smoking, and more. These are just a few examples. Keep in mind that what triggers your symptoms might be different from what triggers someone else’s.
-
You have several breakfast options if you have gastroparesis. Smoothies, oatmeal or other cooked cereals, eggs, yogurt, pureed fruit, and more are all easy to digest.
-
Symptoms of gastroparesis in pregnancy are basically the same as gastroparesis symptoms when not pregnant. You might experience early fullness while eating, bloating or distension, abdominal pain, nausea or vomiting, and fatigue.