If you’re experiencing new, worsening, or ongoing digestive problems, whether constipation, diarrhea, bloating, nausea, reflux, or a combination, you might be wondering what’s up. The digestive tract is a long and winding path, and symptoms can match up with multiple conditions. Your best bet? Take note of what you’re experiencing, how long it’s been going on, and any triggers you’ve noticed–and then talk to a clinician who can help.
When digestive problems crop up, you likely put on your detective hat and start going over the clues. When did the issues start? How severe are they? Do you have any other bodily symptoms?
These are questions you might ask yourself as you create one of those”situation room” evidence corkboards you see on police procedural shows in your mind. You might connect a string between sudden gastrointestinal (GI) issues and foods you ate, pointing to a temporary issue. Or maybe you discover a clue about ongoing or recurring symptoms that warrant further investigation with a clinician who can diagnose you and develop a treatment plan.
If determining the reason for your GI issues feels like having to solve a complex mystery, it’s probably because symptoms can correlate with several conditions, both temporary and chronic. However, some clues and patterns can help you narrow down the possibilities and help you determine your next steps.
In this article, we explore digestive issues, stomach problems, gastrointestinal disease, when to see a provider, and more.
Digestive issues vs. stomach issues vs. gastrointestinal disease
Before we go further, let’s clarify some terms, since the varied wording surrounding symptoms can get a bit confusing. Let’s break it down:
-
Digestive issues: This umbrella term covers symptoms that can appear anywhere from your mouth to your anus. This passageway for nutrients and waste is called the gastrointestinal tract or digestive tract.
-
Stomach issues: This category is limited to a single organ: your stomach, which is located in your upper abdominal cavity. It stores, churns, and digests food with its unique cocktail of acids and enzymes.
-
Gastrointestinal disease: This term covers chronic conditions (rather than acute symptoms) that can affect any part of the GI tract.
Understanding these distinctions can help you describe your symptoms more clearly, avoid unnecessary worry, and better determine when it’s time to seek medical care.
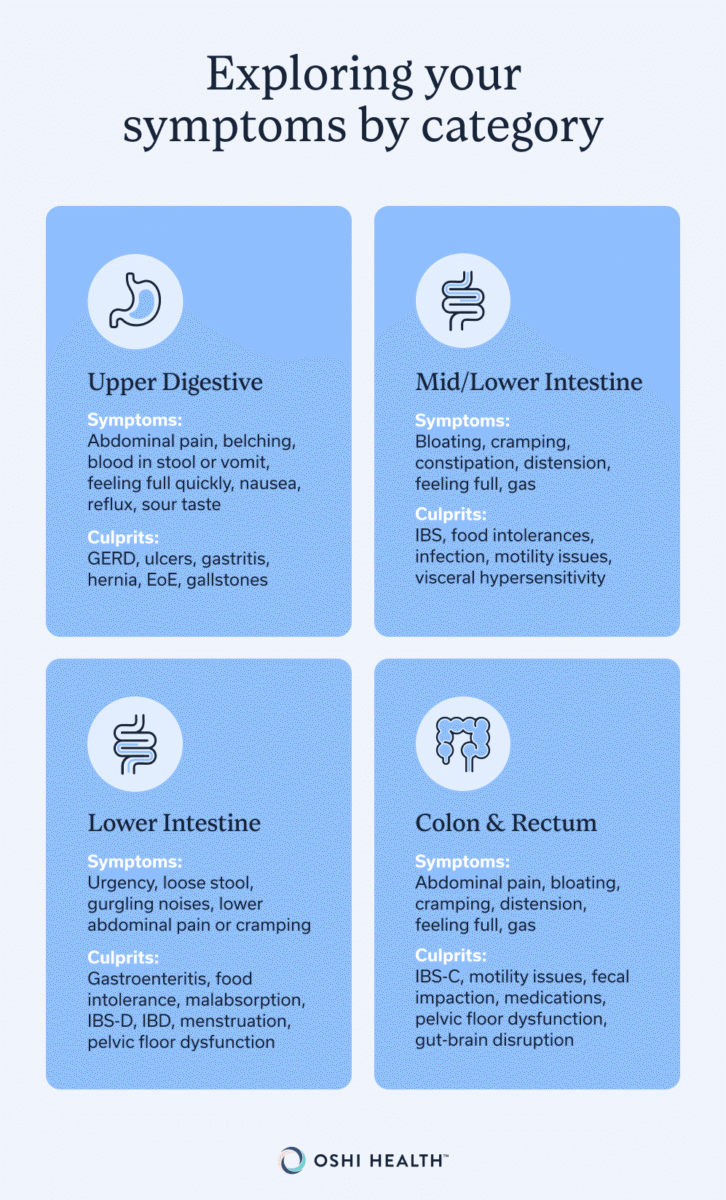
Exploring your symptoms by category
Thinking about your symptoms using the definitions above can help you home in on what might be going on. From there, you can review the more specific categories below to begin narrowing in on potential causes. But just because your symptoms, their timing, and other factors align with one of these categories or individual diseases doesn’t automatically mean you have the condition. That’s why talking to a knowledgeable clinician can be an important step in helping you figure it out.
Upper digestive problems
Upper digestive problems typically involve your stomach and esophagus (food pipe).
Common symptoms:
-
Abdominal pain or discomfort (upper)
-
Belching
-
Blood in your stool or vomit
-
Feeling full quickly
-
Nausea or vomiting
-
Reflux or heartburn
-
Sour or bile taste
Common culprits:
-
Gastroesophageal reflux disease (GERD) or acid reflux: Acid reflux occurs when stomach acid goes in the wrong direction, finding its way from your stomach to your esophagus and sometimes up to your throat. Symptoms may or may not include heartburn. Reflux can occur occasionally from eating certain foods or taking certain medications. But GERD is a chronic form of the issue.
-
Peptic ulcers: These sores that cause burning or pain occur in the lining of the stomach or duodenum (first part of the small intestine). They typically result from taking nonsteroidal anti-inflammatory drugs (NSAIDs) or developing an H. pylori infection.
-
Gastritis: Inflammation of the stomach lining can be caused by several factors, including irritation or infection, and can lead to pain.
-
Hiatal hernia: This type of hernia occurs when part of the stomach pushes through the diaphragm, leading to pain in the mid- to upper-abdominal area.
-
Eosinophilic esophagitis (EoE): This is a chronic inflammatory disease where eosinophils (a type of white blood cell) increase in the esophagus, leading to pain, difficulty swallowing, and other symptoms.
-
Gallstones: Crystallized deposits form in the gallbladder, sometimes blocking bile flow, resulting in upper right-side abdominal pain.
When to see a clinician: Always see a provider if your pain or other symptoms are severe, if you have vomiting that doesn’t resolve, you experience unexplained weight loss, if you notice blood in your stool or vomit, or if your vomit looks like coffee grounds.
Bloating, distension, and gas
Bloating, distension, and gas can involve multiple areas of the digestive tract, especially the mid-to-lower abdominal area. Bloating is the feeling of pressure, fullness, or trapped gas. Distension, however, is visible or measurable swelling. They can occur together or individually, and they may involve gas.
Common symptoms:
-
Bloating
-
Cramping
-
Constipation
-
Distension
-
Feeling full
-
Gas
Common culprits:
-
Irritable bowel syndrome (IBS): IBS is a bowel disorder diagnosis with recognized subtypes (IBS-C, IBS-D, IBS-M), all of which feature abdominal discomfort related to changes in bowel habits.
-
Food intolerance: Several food intolerances are linked to bloating, distension, and gas, including lactose intolerance, FODMAP intolerance, Celiac disease or gluten sensitivity, and more.
-
Infection: An infection can upset the delicate balance of your gut microbiome (the bacteria and fungi that live in your gut), leading to chronic or intermittent bloating, distention, or gas.
-
Gut motility issues: Gut motility is how food and waste move through your digestive tract. When it’s slowed, whether from certain medications or another issue, bloating and other symptoms can ensue.
-
Visceral hypersensitivity: This is a functional issue that means experiencing a lower threshold for GI-tract pain and discomfort. It can occur as part of IBS, inflammatory bowel disease (IBD), or other conditions, including endometriosis, polycystic ovary syndrome (PCOS), uterine fibroids, and more.
When to see a clinician: Talk to a provider if your symptoms of bloating, gas, or distension are severe or don’t resolve, or if they return frequently. Blood in your stool is always a reason to talk to a doctor as soon as possible.
Diarrhea and urgency
If you find yourself frequently heading to the loo for a number two that is soft or runny, the issue is probably something going on with your lower GI tract or nearby structures.
Common symptoms:
-
Diarrhea or loose and watery stool
-
Fecal incontinence
-
Frequent urge to go number two
-
Gurgling or gut noises
-
Lower abdominal pain or cramping during defecation
Common culprits:
-
Gastroenteritis: This inflammation of the GI tract is sometimes referred to as the”stomach flu” and can occur from bacteria, viruses, or parasites. Nausea, vomiting, diarrhea, and lower abdominal pain are common symptoms.
-
Food poisoning: This type of gastroenteritis results from eating contaminated food.
-
Food intolerance: Several food intolerances are linked to diarrhea, including lactose intolerance, FODMAP intolerance, Celiac disease or gluten sensitivity, and more.
-
Malabsorption issues: Impaired digestion or difficulty absorbing nutrients can also lead to diarrhea.
-
IBS: IBS has several types, including a form that typically leads to diarrhea (IBS-D).
-
IBD: This umbrella term includes Crohn’s disease and ulcerative colitis, and both can cause abdominal pain, diarrhea, and other GI symptoms.
-
Menstruation: During your period, rising prostaglandin levels stimulate uterine contractions. But sometimes the prostaglandins also stimulate GI tract muscles, causing diarrhea, cramping, and more.
-
Pelvic floor dysfunction: Your pelvic organs are held in place by supportive muscles called the pelvic floor. Sometimes these muscles become tight or weak or have difficulty coordinating, leading to fecal incontinence.
When to see a clinician: You should talk to a medical professional if your diarrhea is severe or ongoing or if you notice blood in your stool, which is a medical emergency.
Constipation and sluggish gut symptoms
Sometimes GI issues involve an inability to go, having bowel movements that leave you feeling like you still need to do a number two, or going several days without a bowel movement when that’s not normal for you.
Common symptoms:
-
Abdominal pain
-
Bloating
-
Cramping
-
Constipation
-
Distension
-
Feeling full
-
Gas
Common culprits:
-
IBS: IBS has several types, including a form that typically leads to constipation (IBS-C).
-
Gut motility issues: Slowed gut motility can lead to less frequent bowel movements.
-
Fecal impaction or bowel obstruction: A fecal impaction is when a hard mass of stool gets stuck and prevents or limits bowel movements. A bowel obstruction is a blockage somewhere in the intestine caused by something else, such as scar tissue or a tumor, that prevents stool, fluid, and even gas from passing.
-
Medications: Some medications, including opioids, iron supplements, antidepressants, and more, can cause constipation as a side effect.
-
Pelvic floor dysfunction: When your pelvic floor muscles are tight, can’t relax, or have trouble coordinating, constipation can occur.
-
Gut-brain disruption: Your gut and brain communicate via the gut-brain axis, but sometimes this communication gets disrupted, leading to slowed digestion or chronic constipation.
When to see a clinician: Talk to a provider if you have severe symptoms. Seek medical attention right away if you cannot go number two or pass gas at all or if you notice blood in your stool.
5 questions to consider regarding your GI symptoms
If you’re not sure which of the above categories your symptoms fall under, five questions can be helpful in making the determination. Your answers can be especially helpful when you’re talking to a clinician about what you’re experiencing.
-
Where are your symptoms located? Can you pinpoint where your symptoms are in your GI tract? Are they occurring in your mouth, throat, upper abdomen, lower abdomen, etc.? And are they limited to just one side?
-
How long have your symptoms been going on? Have your symptoms been present for 24 hours, a few days, a week, a month, or longer?
-
What are they and when do your symptoms occur? Can you name your specific symptoms (e.g., pain, bloating, heartburn, diarrhea, constipation, etc.), and when does each symptom crop up (e.g., after eating, while sleeping, upon waking, etc.?)

-
Can you identify any symptom triggers? Do your symptoms develop after you’ve eaten specific foods, during or after travel, after taking antibiotics, in response to specific activities, etc.?
-
Have you noticed any stool changes? If so, note the color and consistency, whether you see blood or mucus, and whether you’re having diarrhea, constipation, pain, or other symptoms in relation to going number two. Use the Bristol Stool Chart to note what your stool looks like.
Working with a healthcare provider
As you can see, diagnosing GI issues can take a lot of detective work, but you don’t have to figure out what’s going on all by yourself. The team of experts at Oshi Health can help by taking a multidisciplinary approach.
Your care team might include a GI provider (a nurse practitioner or physician associate), a GI registered dietitian, and/or a gut-brain specialist or psychologist, all overseen by board-certified gastroenterologists. They collaborate to help you get to the bottom of your symptoms and develop a treatment plan that’s tailored to you.
Key takeaways
-
When digestive or stomach issues crop up, note the symptoms, their severity, timing, and duration, and any triggers.
-
These notes can offer clues about whether you’re experiencing a temporary issue from a meal or an acute illness, or whether you might have a chronic condition.
-
Either way, you don’t have to do the detective work on your own. Oshi Health can help.
FAQ
-
The digestive tract extends from your mouth to your anus, so any symptom that occurs along your GI tract is considered a digestive issue, including acid reflux, stomach pain, diarrhea, constipation, bloating, excessive gas, and more.
-
If your digestive system feels”messed up,” the situation may be temporary and resolve on its own. However, if your symptoms continue, you should talk to a knowledgeable clinician who can help explore your symptoms and get to the root cause so you can start feeling better.
-
Medical literature does not list four specific signs of a poorly functioning digestive system. Ultimately, if you are experiencing symptoms that affect your digestive tract, talk to a clinician who can help.
-
Some of the most common diseases of the digestive system include GERD, IBS, Crohn’s disease, ulcerative colitis, Celiac disease, gallstones, diverticular disease, peptic ulcers, gastritis, and liver disease.
-
Sometimes digestive issues come on suddenly because of something you ate, an illness or infection, starting your period, and more. If your symptoms don’t resolve, are severe, or you notice blood in your stool or vomit, you should talk to a medical professional right away.
Oshi is your partner in digestive health
Feel like your digestive concerns are running your life? You’re not alone—and we’re here to help you find lasting relief.
Oshi Health GI providers, gut-brain specialists, and registered dietitians work together to address your symptoms and find solutions that actually work for you.