Everyone burps…but what does it mean when you burp a little too much? Excessive burping can be the result of swallowed air, reflux, gut sensitivity, belching disorders, and more. Figuring out the type of burps you’re experiencing is the key to treating them effectively.
As embarrassing as it might feel to let out a belch in a work meeting or in that awkward silence during a first date, burping now and then is totally normal! Burping excessively, to the point it disrupts your daily life, is not normal. The uncomfortable side effects that often show up alongside excessive burping—bloating, reflux, nausea, constipation— certainly aren’t pleasant, either.
Luckily, excessive burping is typically treatable once you pinpoint the cause. This guide explains common causes and practical ways to burp less (including both short-term and long-term strategies that actually stick).
Excessive burping: What counts as “excessive” and why it happens
Between burping and farting, it’s considered normal to pass gas up to 21 times a day. However, even this number of burps can feel excessive if it’s interrupting your life on a regular basis. In general, burping is considered excessive if it’s:
- Disruptive
- Frequent
- Paired with symptoms like pain, nausea, or weight loss
But let’s back up a second. Why do burps happen in the first place? Burping is how your body releases gas. It’s a normal bodily function—until it’s not.
“Think of burping as a pressure-release valve,” says Omar Khokhar, MD, board certified gastroenterologist. When too much air collects in the stomach or esophagus, it’s released as a burp.
There are two different ways burps happen. These are:
- Gastric belching (from within the stomach): This happens when air accumulates in your stomach, often from gas produced during digestion. As your stomach expands, the vagal reflex kicks in, and the lower esophageal sphincter (a ring-shaped muscle at the bottom of your food tube) relaxes. Then, air moves up and out as a burp.
- Supragastric belching (from above the stomach): You can also burp out air that’s held in your esophagus. This happens when air is pulled into the esophagus via a quick inhale or throat movement. The air is immediately expelled before it has the chance to enter your stomach. (When it happens excessively, this type of burp is considered a behavioral disorder.)
“The key distinction here is that gastric belching is a volume issue, and supragastric belching is a behavior and reflex loop,” says Dr. Khokhar. Because these types of burps have different causes, they also have completely different solutions.
If you’re burping dozens (or even hundreds) of times per day, then you might have a problem with either swallowing too much air or producing too much gas.
Some health conditions and factors that might be at play include:
- Anxiety and stress
- Chewing or drinking habits
- Food and drink triggers
- Gastritis
- Gastroparesis
- Gut sensitivity
- H. Pylori infection
- Post-surgery anatomical changes
- Reflux
- Small intestinal bacterial overgrowth (SIBO)
Getting to the bottom of why you’re burping so much can take some investigation, but you don’t have to do all the detective work on your own. Working with a healthcare provider who specializes in gastrointestinal conditions, like those at Oshi Health, can help you identify and treat your burping pattern, and not just stop the symptom.
Why am I burping so much? Everyday habits that add air
Swallowing too much air (also called aerophagia) is the usual suspect when it comes to burping, according to Dr. Khokhar. “There’s a net effect here. When excess air goes down, the body has to offload it.”
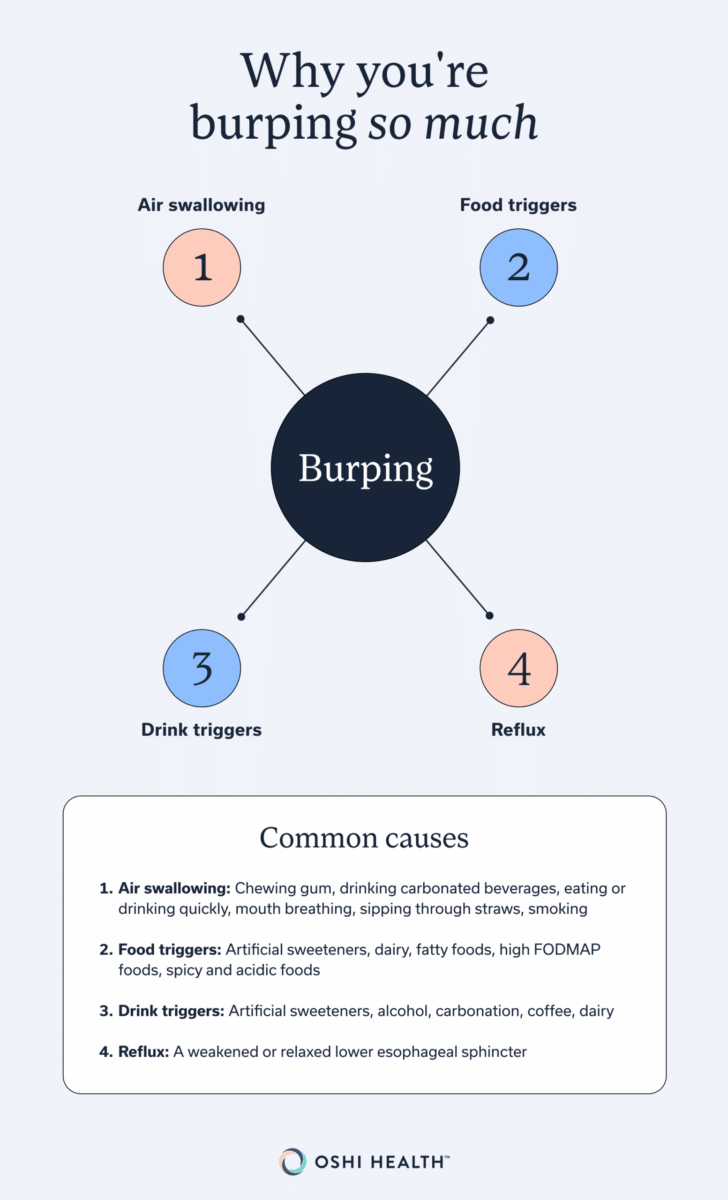
The tricky part is that many people don’t even realize they’re swallowing air. Some habits that can increase how much air you swallow include:
- Chewing gum
- Drinking carbonated beverages
- Eating or drinking quickly
- Large gulps
- Loose dentures
- Mouth breathing
- Sipping through straws
- Smoking or vaping
- Talking while eating
Anxiety and stress can also lead to swallowing air, often without you even noticing. When you’re stressed, you might unconsciously hold your breath or swallow more frequently.
If your burps are due to swallowed air, then you might also feel bloated or constipated, or your belly might be visibly swollen.
Potential treatments
If swallowed air is the driver of your excessive burping, then some solutions may include:
- Cutting out carbonated drinks
- Eating slowly
- Keeping your mouth closed while chewing
- Skipping chewing gum and using straws
Why do I burp so much after eating? Common triggers and patterns
That six-bean chili or extra glass of wine after work might be the culprit behind your burps. Certain foods and drinks can make you burp more than others.
Common food and drink triggers include:
- Artificial sweeteners: Often found in sugar-free candy and gum, these can alter gut bacteria, be difficult to digest, and produce gas.
- Beer, wine, and liquor: Alcohol can relax the sphincters in your esophagus and stomach, bringing air back up as a burp. Carbonation in alcoholic drinks also adds gas.
- Carbonation: This one seems pretty obvious, but it’s worth mentioning again. The gas bubbles in fizzy drinks can lead to trapped air.
- Coffee: Your morning brew might also bring on burps. Coffee can stimulate stomach acid, and the caffeine it contains can relax your lower esophageal sphincter so that air escapes more easily.
- Dairy: If you’re lactose intolerant, certain dairy foods can trigger gas and burping.
- Fatty foods: High-fat foods can delay gastric emptying, leading to a buildup of gas in your stomach.
- High FODMAP foods: Some foods (like onions, beans, and garlic) are high in fermentable carbohydrates and can produce extra gas during digestion.
- Spicy and acidic foods: These can worsen reflux symptoms for people who are sensitive.
It’s not only down to what you eat. How you eat can cause burping, too. Eating and drinking patterns that trigger burping include:
- Late meals: Eating late at night can worsen reflux symptoms, which may increase burping and other gastrointestinal (GI) symptoms overnight.
- Large meals: Eating a big meal can slow down stomach emptying and increase burping.
- Sudden changes in your diet: Diet changes like eating more fiber or adding a new protein powder can increase gas.
Potential treatments
If food and drink are triggering your burps, then a trial of nutrition changes can help. For example, the low FODMAP diet can reduce burping for some people.
A GI registered dietitian, like those who work with Oshi Health, can recommend and guide you through dietary changes to identify triggers and create a nutritional plan that addresses your symptoms.
Burping a lot with heartburn or sour taste: Reflux and GERD clues
If your burps have a sour taste, burn your throat, or bring up an acidic liquid (lovely, we know), then this could be a sign of reflux.
Reflux-related burping happens when acid or non-acid reflux triggers the lower esophageal sphincter to relax. Air escapes upward—along with some of your stomach contents.
If you have reflux, you may also make yourself belch because this relieves symptoms. Reflux burps can sometimes (but not always) be paired with symptoms like:
- Chest tightness
- Difficulty swallowing
- Heartburn
- Nausea
- Regurgitation
If you have reflux burps, then your burps (and any accompanying symptoms) might worsen after meals, when you’re lying down, or after you consume trigger foods or drinks.
Reflux burps can be sneaky and don’t always come with classic acid reflux signs. If you have non-acid reflux, then instead of feeling a burning liquid alongside your burps, you might get a hoarse voice or coughing.
Potential treatments
If reflux is part of the equation, then the following might help, according to Dr. Khokhar:
- Avoiding lying down within three hours of eating
- Eating earlier dinners
- Eating smaller meals
- Drinking less alcohol
- Eating fewer fatty foods and late-night snacks
Your GI provider may also prescribe medications, like proton pump inhibitors (PPIs). This is most effective for acid reflux (when you regurgitate a sour liquid), and may not work as well for burps related to non-acid reflux (when you tend to cough and might have a hoarse voice).
Excessive belching disorders: When it’s more about air movement than digestion
A recent study found that 1.5 percent of its 10,000 participants had a belching disorder. These are gut-brain disorders that cause excessive burping—sometimes hundreds or even thousands of times per day.
A belching disorder is diagnosed if someone experiences:
- Belching is severe enough to affect their usual activities
- Severe belching over more than three days a week for at least three months
It’s tough to put an exact number on what counts as an excessive belching disorder. Some scientists have proposed 13 or fewer supragastric burps in 24 hours as normal, and anything more as excessive. However, it really comes down to how much these burps disrupt your daily life and how irritating they are to you.
Belching disorders are classified by the different types of burps that are predominant. These burps can be one of two types:
- Excessive gastric belching: Gas from the stomach is burped out repetitively. This is often associated with gastroesophageal reflux disease (GERD) or eating habits.
- Excessive supragastric belching: Gas from the esophagus (not swallowed fully into the stomach) is burped out repetitively. Unlike gastric belching, this is a learned behavior. It’s commonly associated with anxiety and obsessive-compulsive disorder (OCD).
“[Supragastric belching] is one of the most underdiagnosed but fixable GI issues,” says Dr. Khokhar. “This is a learned, subconscious behavior, not a stomach problem.”
Some clues that you might be dealing with supragastric belching are if your burps are worse when you’re talking, stressed, or hyper-focusing on your symptoms, and go away when you’re sleeping or distracted.
Potential treatments
Excessive gastric belching is treated by addressing the underlying cause, such as reflux or food sensitivities.
For excessive supragastric belching, the solution is often behavioral training and breathing techniques, not medication. “Awareness is step one,” says Dr. Khokhar. “Most people don’t realize they’re doing it.”
Effective treatments for supragastric belching include:
- Breathing techniques, such as belly breathing
- Cognitive behavioral therapy (CBT)
- Hypnosis
- Speech therapy
Gut sensitivity: bloating, pressure, and burping
For some people, normal amounts of gas in their stomach can feel excessive, resulting in frequent burps. “This is the gut-brain axis overreacting,” explains Dr. Khokhar.
Gut sensitivity (also called visceral hypersensitivity) is common in people with irritable bowel syndrome (IBS), indigestion, anxiety, or who are under high stress.
Potential treatments
If your gut sensitivity is high, then treatments might include:
- A low FODMAP diet, if you’re also experiencing bloating
- Neuromodulator medications
- Stress management
Diagnosis and testing: How clinicians evaluate excessive burping
As you can see, there’s a lot happening behind the scenes when you burp. Your healthcare provider’s first step is usually to get a history of your symptoms. They may ask questions like:
- Do you burp more at certain times of day?
- Have you noticed links between burping and what you eat or drink?
- Does your stress level affect your burps? Do you have a history of anxiety?
- Do you have reflux symptoms, like heartburn or regurgitation?
- Do you feel bloated? Constipated?
- Have your bowel movements changed?
- How many times do you burp per day?
- How is burping affecting your quality of life?
They’ll also review your medications and supplements, because these can sometimes irritate your stomach or affect how fast food moves through your digestive tract.
If your symptoms persist after making lifestyle changes (like giving up seltzer and midnight snacking), then your healthcare provider might order some diagnostic tests.
Tests for excessive burping can include:
- Breath testing: There are different types of breath tests, some of which can diagnose H. pylori infection.
- Medication trial: If reflux is suspected, then a clinician might have you try a medication like PPIs for a period of time, to see if that helps your symptoms.
- Stool test: Pooping in a medical jar might not be fun, but it can be enlightening. Stool tests can reveal H. pylori, among other infections.
- Esophageal manometry: This test looks at what’s happening with the muscles in your esophagus and stomach during a burp, and can differentiate supragastric belching from gastric belching.
- Upper endoscopy: This test is reserved for alarming symptoms (like vomiting or unexplained weight loss), or if your symptoms don’t get better over time. It involves sending a (very tiny) camera down your throat to view your esophagus, stomach, and top of your small intestine. Don’t worry—you’ll get anesthesia.
How to stop burping: Quick tips for relief vs long-term solutions
Treatments for excessive burping depend on the type of burps you’re experiencing and what’s actually causing them.
However, there are some things you can do in the short-term to get relief fast. Try to:
- Avoid gulping liquids
- Avoid gum and hard candies
- Eat slower
- Keep a simple log for one week (record your meals, drinks, stress, symptoms, and timing)
- Pause during meals to chew thoroughly
- Practice belly breathing
- Quit carbonated beverages
- Take a gentle walk after meals
To make this feel more manageable, focus on the top one or two potential triggers (like carbonation or speed eating) that you can change this week. Next week, reflect on how you feel and target another trigger.

Long-term relief from excessive burping comes from eliminating those pesky “air-adding” habits, as well as treating your underlying cause. Consider working with a multidisciplinary GI care team, such as the GI providers, registered dietitians, and gut-brain specialists at Oshi Health, to discuss diagnosis and treatment.
When to seek care (red flags)
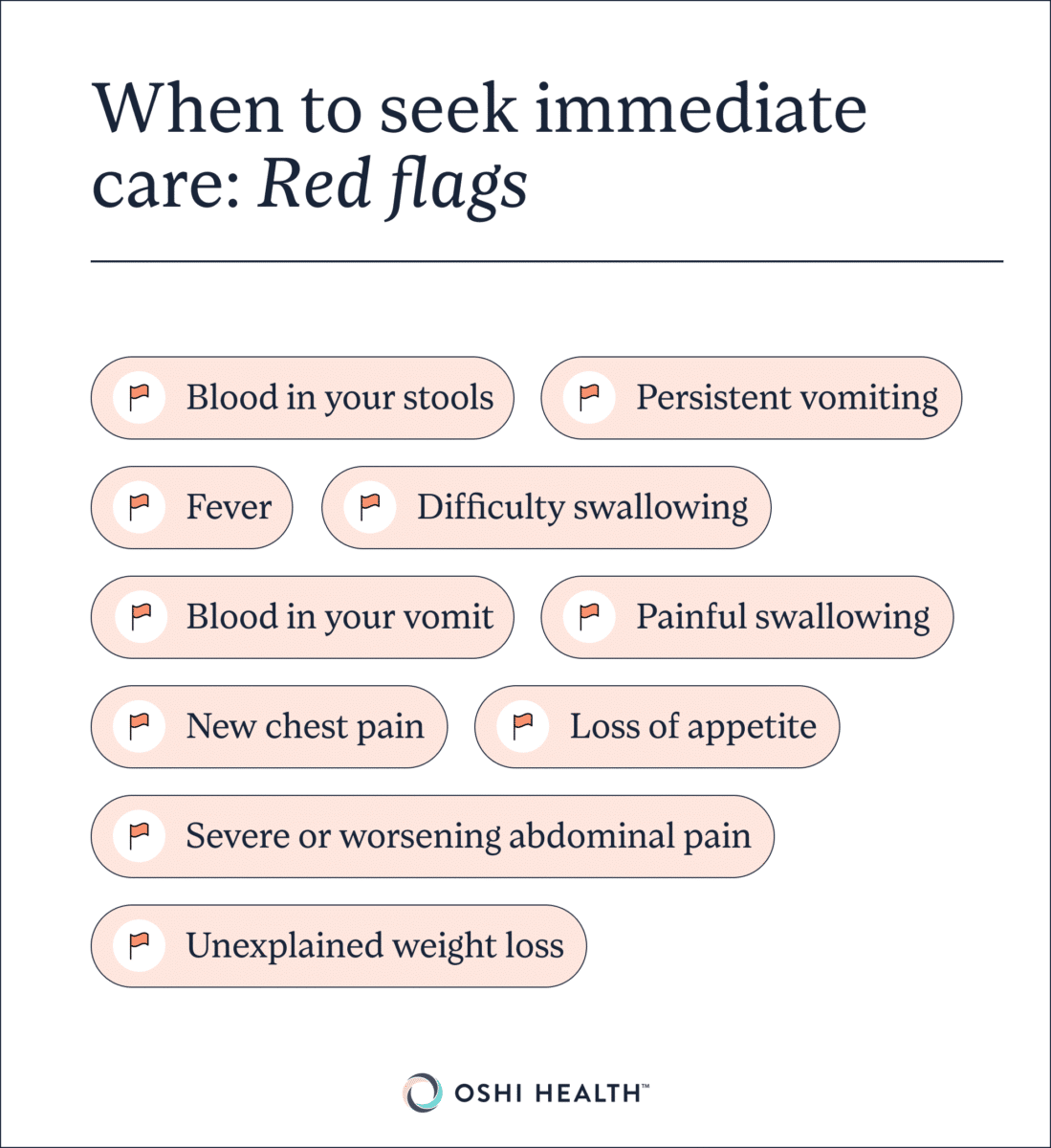
There are a few red flags that should prompt you to see a healthcare provider, stat. These include:
- Blood in your stools (can also look black or tarry)
- Blood in your vomit (can also look like coffee grounds)
- Difficulty swallowing
- Fever
- Loss of appetite
- New chest pain
- Painful swallowing
- Persistent vomiting
- Severe or worsening abdominal pain
- Unexplained weight loss
Ultimately, it’s worth talking to a healthcare provider if any of your symptoms rapidly worsen, wake you up from sleep, or significantly reduce your quality of life.
Working with a healthcare provider (what to bring to a visit)
Oshi’s multidisciplinary experts take the time to listen and get to know you, so they can create a personalized treatment plan. It can be helpful to do some prep work before your first visit to make it as successful as possible.
Some things to share with your healthcare provider include:
- Associated symptoms: Keep a list of any symptoms that accompany your burps, such as heartburn, bloating, constipation, nausea, upper belly pain, bowel movement changes, vomiting, and more.
- Burping patterns: Bring a record of when your burping happens, how often it happens, and what makes it better or worse. It’s okay to guesstimate—your provider just wants to get the general picture.
- Diet: Keep a note of the types of foods and drinks you typically consume, especially any carbonated drinks, gum or mints, alcohol, and any recent changes to your diet.
- Medications: Share all your medications and supplements.
At your appointment, ask about the most likely cause for your pattern of burping, and what to try first to resolve it. You’ll also want to ask what timeline to expect for improvement.
If your symptoms continue, then it’s worth discussing whether further testing is appropriate.
The takeaway
- Excessive burping is often due to swallowed air, reflux, or specific gut sensitivities.
- Burping a lot can also be a behavioral issue, sometimes driven by anxiety, stress, or OCD.
- The fastest improvement usually comes from slowing meals and cutting carbonation.
- If your symptoms don’t go away (or red flags show up), then a clinician can help confirm the cause and build a targeted treatment plan.
Frequently asked questions (FAQs)
What is the cause of excessive burping?
Excessive burping is usually due to swallowing too much air, but it can be caused by lots of things: reflux, lactose intolerance, gut sensitivity, belching disorders, anxiety, infections, and more.
Is burping an anxiety symptom?
Yes, burping can be a symptom of anxiety. You might swallow more air or hold your breath unconsciously when you’re anxious. Excessive supragastric belching (a type of belching disorder) has also been linked to anxiety.
What should I take for excessive burping?
There’s no specific medication for excessive burping. If your burping is due to GERD, then your healthcare provider might prescribe a PPI.
When should I be worried about burping?
The good news is that most people don’t need to be worried about burping. It’s normal to burp; even a lot of burping is generally harmless (albeit uncomfortable) and possible to treat. If, however, you burp so much that it’s disrupting your life on a regular basis, then it’s worth talking to a healthcare provider. You should also be concerned if your burping is paired with symptoms like weight loss, difficulty swallowing, or vomiting.
What is the best home remedy for excessive gas?
If you’re feeling gassy, start with home remedies such as slowing down your meals, cutting out carbonated beverages, belly breathing, and tracking your diet and symptoms for triggers.