Pain in your upper right abdomen? Is your urine darker than usual? Have you been feeling more gassy lately? All three might be signs of gallbladder issues. Read on to learn more about the symptoms of gallbladder problems, other conditions that can cause these symptoms, and what to do if these symptoms strike.
Gallbladder problems aren’t talked about as often as some other GI conditions, but they are quite common. 20 million Americans have gallbladder disease, and even more have gallstones (one study places gallstone prevalence at 6 percent of the world’s population). However, only about one in ten people with gallstones will develop symptoms, and a lot of them overlap with other gastrointestinal (GI) conditions, making gallbladder issues tricky to diagnose. All of this begs the question, “What are the first signs of a bad gallbladder?”
The first symptoms will vary depending on the underlying condition. Sometimes, they are minor, such as feeling extra bloated or passing more gas than usual. Other times, they’re more severe, such as severe pain in the abdomen or intense nausea. The good news? Many gallbladder problems are treatable, especially when caught early. Ahead, we’ll investigate the warning signs of a bad gallbladder, when to seek care, and what might be causing gallbladder issues in the first place.
Gallbladder basics
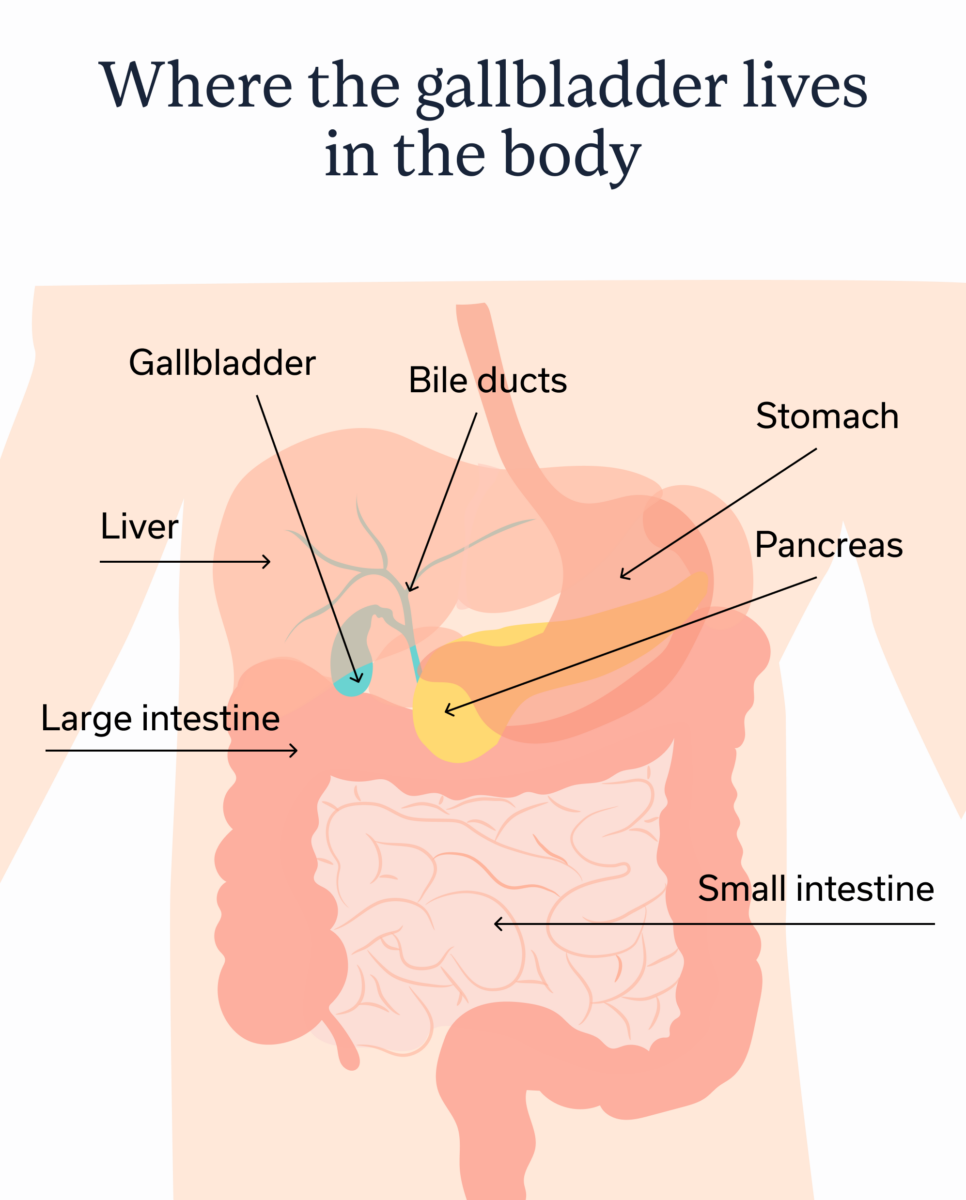
Let’s start with anatomy 101: what even is the gallbladder? It’s a pear-shaped organ that rests under the liver. Because the liver is such a good neighbor, it shares the bile it produces with the gallbladder. The gallbladder then stores and concentrates that bile.
When the small intestine digests food, the gallbladder releases the bile, and it travels to the small intestine via a tube known as the common bile duct. That bile helps with the absorption of fatty acids, cholesterol excretion, and even has antimicrobial properties. Basically, your gallbladder supports the healthy function of the digestive system and metabolism.
“A’bad gallbladder’ is one that is not working properly or is causing pain, due to gallstones, inflammation, or decreased gallbladder function,” says Gabriella McCarty, DNP, MSN, NP-C, a GI provider at Oshi Health. Problems may also occur if there’s a blockage or other issue in the common bile duct.
What are the first signs of a bad gallbladder?
“The most common early sign is right upper abdominal pain,” says McCarty, “especially after eating fatty, fried, or greasy foods.” Gallbladder-related pain is a bit of a homebody, meaning it usually stays in the right upper stomach—unless it’s severe. In those cases, it can radiate to the upper back or shoulder.
Beyond potential travel to the back and shoulder, gallbladder pain is usually localized, meaning it won’t move to other parts of the abdomen or digestive tract. The pain can go away, but it usually returns and often has clear triggers. McCarty explains, “Gallbladder pain usually occurs after eating fatty meals, localized to the right upper abdomen, and may radiate to the back or shoulder. This pattern is less common with reflux or ulcers.”
While pain is the most common first sign, someone may also experience gas, nausea, or abdominal discomfort, especially after meals, as an initial symptom.
Early signs of a bad gallbladder can vary in intensity. Sometimes, they require emergency medical attention. Other times, someone may write them off as a fluke or mild indigestion. What all signs share, however, is that they typically come and go—and they require medical attention.
Signs of gallbladder issues
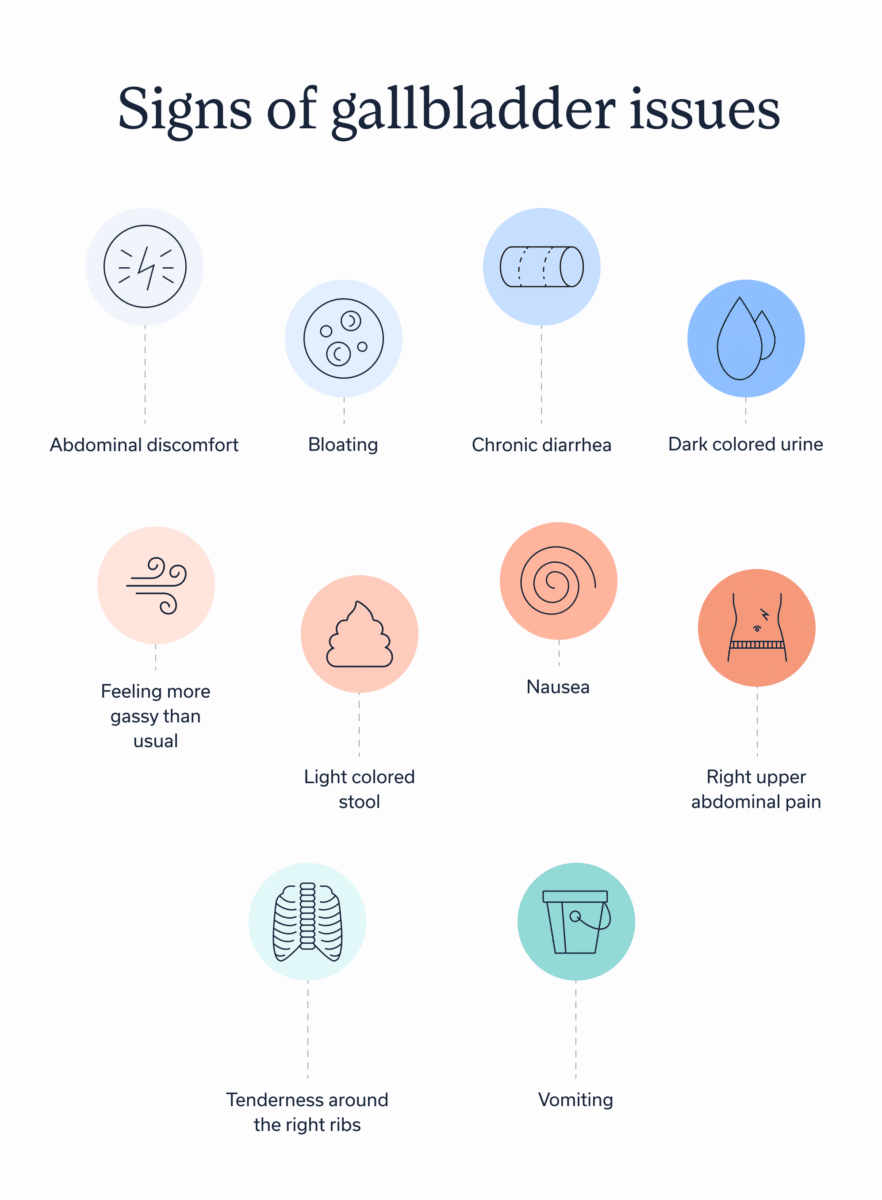
Gallbladder symptoms vary quite a bit, depending on the underlying cause. Some of the most common include:
- Abdominal discomfort
- Bloating
- Chronic diarrhea
- Dark colored urine
- Feeling more gassy than usual
- Light colored stool
- Nausea
- Right upper abdominal pain
- Tenderness around the right ribs
- Vomiting
Weird signs of a bad gallbladder
Sometimes, gallbladder symptoms aren’t what you might expect. Less obvious signs of a bad gallbladder may include:
- An indigestion-like sensation that can be predicted. Typically, this occurs after eating something fatty, fried, or greasy (think: French fries, a burger, or a funnel cake).
- Burping or farting more than usual
- Feeling overly full
- Pain in the upper back or shoulder
- Pain that wakes you up in the night, especially after a late meal
- Symptoms that don’t improve with antacids
Gallbladder problems: What might be going on
So, what actually causes a bad gallbladder? There are many potential culprits. The most common are cholecystitis (aka gallbladder disease) and gallstones, though others exist, too.
Gallbladder disease
Gallbladder disease is an umbrella term for conditions that affect the structure or function of the gallbladder, often involving problems with bile storage or flow. One of the most common types of gallbladder disease, known as cholecystitis, occurs when the gallbladder becomes inflamed. Cholecystitis can be acute (sudden and severe) or chronic (long-lasting). It can occur with or without gallstones, which we’ll get to in a minute.
Chronic cases aren’t always symptomatic, but when they are, there’s usually a dull pain in the upper right abdomen. Sometimes, symptoms may include increased gas, bloating, nausea, and possibly vomiting. Without treatment, symptoms may become more severe and episodes more frequent.
Acute cholecystitis leads to more serious symptoms, such as fever or vomiting, and the upper right abdominal pain becomes much more severe and typically lasts at least six hours. Chronic cases may evolve into acute ones, or cases may be acute from the start. If left untreated, acute cholecystitis can lead to serious complications, like sepsis and possibly death.
Gallstones
Gallstones are hard deposits that can be as small as a grain of salt or as big as a golf ball. They can occur in the gallbladder or the common bile duct. Most don’t cause symptoms, and these are referred to as”silent gallstones.” When they do trigger symptoms, they can be serious if left untreated.
There are two main types of gallstones: cholesterol stones and pigment stones. As the name suggests, cholesterol stones are cholesterol deposits that can form due to a high-cholesterol diet. Pigment stones occur when there’s too much bilirubin, a yellowish pigment, in the bile. They’re often caused by blood disorders (like sickle cell anemia), liver disease, or infections.
Somewhere between 10 and 15 percent of Americans have gallstones. While gallstones can happen to anyone, there are some factors that increase the risk of developing them:
- Being female, especially when there is extra estrogen in the body due to pregnancy, hormone replacement therapy, or birth control
- Being of Latin American or Indigenous American descent
- Having a family history of gallstones
- Having certain conditions, such as diabetes or Crohn’s disease
- Being overweight or obese
Other gallbladder problems
It is possible to experience other gallbladder problems, including:
- Acalculous gallbladder disease: A form of gallbladder inflammation that occurs without gallstones, most often as an acute and potentially life-threatening condition, particularly in critically ill individuals.
- Congenital defects of the gallbladder: Conditions where there’s a structural or functional issue with the gallbladder. These are present at birth.
- Gallbladder cancer: A rare condition where cancerous cells are present in the gallbladder.
- Gallbladder polyps: Abnormal tissue growths in the gallbladder that are often asymptomatic but can sometimes cause symptoms or, in rare cases, be cancerous.
- Gangrenous cholecystitis: A severe complication of acute gallbladder inflammation in which reduced blood flow causes gallbladder tissue death.
- Perforated gallbladder: A rare but life-threatening complication of acute gallbladder disease, where the gallbladder ruptures and leaks bile.
- Porcelain gallbladder: An uncommon condition where calcium builds up on the inner gallbladder wall, making it hard and brittle–and sometimes increasing the risk of gallbladder cancer.
Gallbladder attack vs everyday stomach issues: How to tell the difference
Nausea, bloating, and even upper right abdominal pain don’t just stem from the gallbladder. Everyday stomach issues, such as indigestion after a particularly heavy meal, and other GI conditions can lead to similar symptoms. Telling them apart can be difficult, but it’s also crucial since gallbladder attacks often require prompt medical attention.
| Cause of upper abdominal pain | How it typically feels | Where it’s located | Triggers / causes |
| Gallbladder problems | Severe and persistent, though it can come and go | Upper right abdomen | Likely to occur after a heavy meal or at night |
| Acid reflux and GERD | A burning sensation | The chest | Typically, after eating, though other habits may cause symptoms too |
| Gastritis | A gnawing pain, indigestion, or uncomfortable fullness | Below the chest but above the belly button | Gastritis, or inflammation of the stomach lining, has many triggers, from bacterial infections to drinking too much alcohol |
| Peptic ulcers (stomach ulcers) | Dull or burning | Below the chest but above the belly button | This sore in the stomach lining is often triggered by bacteria or long-term use of anti-inflammatory drugs (NSAIDs), such as ibuprofen. It may also stem from high stress, smoking, or excessive alcohol. |
Diagnosis and testing: How gallbladder disease is confirmed
To diagnose what’s causing symptoms, a healthcare provider will ask about what the pain feels like, when it appears, and how long it lasts, as well as more general questions about your medical history and what medications you take. They will also conduct a physical exam where they’ll feel for tenderness in the upper right abdomen and assess for any other physical symptoms.
This initial assessment can be done by a primary care provider, though they’ll refer you to a GI specialist , such as a gastroenterologist or GI-trained physician’s assistant or nurse practitioner, if they suspect gallbladder problems. Alternatively, you can skip the primary care appointment and see a GI specialist, like those available at Oshi Health, first.
The GI specialist may order lab tests that can show signs of inflammation or other infection markers. They may also order imaging to locate gallstones or other issues.
When it comes to gallbladder concerns, screening from an expert is essential because gallbladder disease can be difficult to diagnose. “Gallbladder disease doesn’t always show up as classic right upper abdominal pain, and normal labs do not always rule it out,” explains McCarty, “Persistent symptoms deserve evaluation, even if imaging is normal initially.”
When to seek emergency care
Gallbladder problems can be serious. Seek emergency care if experiencing:
- Chills
- Dark urine
- Feeling faint or weak alongside other symptoms
- Fever, even a low-grade one
- Jaundice, which is a yellowing of the skin or whites of the eyes
- Light colored stools
- Severe, debilitating pain, especially if it lasts more than a few hours
Treatment options: What helps
When it comes to gallbladder treatment, we have a lot of good news. First, most gallbladder problems are highly treatable, especially if caught early. Second, if someone has gallstones but no symptoms, they don’t require treatment. Third, some gallbladder pain may even go away on its own–though it is also likely to appear again without treatment.
The recommended treatments depend on the cause, and a gallbladder treatment plan might include lifestyle changes, medications, and/or surgery.
First up, lifestyle treatments. When experiencing gallbladder problems, it’s important to stay hydrated (which helps with overall digestion) and to avoid heavy or fatty foods that may make symptoms worse. Since cholesterol can cause gallstones, you’ll especially want to avoid high-cholesterol foods (think: egg yolks, meat, shrimp, and whole-fat dairy products) or enjoy them in moderation.
When pain is moderate to severe, medications can help. If a bacterial infection is present, a GI provider will prescribe antibiotics. No matter the cause, they may also recommend prescription or over-the-counter medications that help with pain or other symptoms. In severe cases, someone may also receive fluids or pain medications via an IV.
When symptoms are severe or keep coming back, a GI provider may perform a cholecystectomy, a surgery to remove the gallbladder. This is done under anesthesia and may require some recovery time.
Before you panic, the gallbladder is not an essential organ, and people can live normally without it. After the surgery, bile flows directly from the liver into the small intestine instead of being stored in the gallbladder.
Working with a healthcare provider
Treating a gallbladder problem can be tricky, which is why it’s important to work with an experienced GI provider. At Oshi Health, our team can assess symptoms and order the right tests, which is often a combination of bloodwork and imaging. Once there’s a diagnosis, our GI providers can help manage symptoms and can coordinate next steps, such as surgery or medications, when required.
Key takeaways
- Early warning signs of a bad gallbladder can run the gamut. Sometimes, they include severe upper abdominal pain and vomiting. Other times, they may be more subtle, such as feeling gassier or more bloated than usual.
- Gallbladder pain typically follows a pattern, stays local to the upper right abdomen, and may be triggered by meals.
- Certain red flags, such as a fever, dark urine, jaundice, or debilitating pain, require immediate medical attention. Any other signs merit a visit to a GI provider.
- Working with a skilled GI provider, such as the team at Oshi Health, can help you identify what’s causing symptoms and create a comprehensive treatment plan.
-
Weird, or unexpected, symptoms of gallbladder problems include pain in the upper back, an indigestion-like sensation, burping or farting more than usual, and feeling overly full. These symptoms often follow a specific pattern and will reoccur if stemming from a bad gallbladder.
-
The five Fs of gallbladder disease refers to a mnemonic device meant to describe the type of person who is most likely to experience cholelithiasis. Basically, it suggests that those who are female, around the age of 40, are able to have children, have fair features, and are overweight or obese are the most likely to have gallbladder disease. While this is fairly accurate, gallbladder disease is becoming more common in younger populations, leading some to suggest replacing the “F” for “forty” with “family history of the disease.”
-
Your gallbladder is likely ok if you aren’t experiencing severe upper stomach pain, nausea, fever, chills, or jaundice, or any other symptoms of gallbladder issues. If in doubt, contact a healthcare provider, such as your primary care provider or a GI specialist.
-
When someone has gallbladder problems, their stool is often lighter in color. Some describe the color as similar to clay.
-
Cholesterol is one of the main causes of gallstones. That means eating a lot of high-cholesterol foods, like egg yolks, meat, and whole fat dairy products, may trigger gallbladder attacks.
Oshi is your partner in digestive health
Feel like your digestive concerns are running your life? You’re not alone—and we’re here to help you find lasting relief.
Oshi Health GI providers, gut-brain specialists, and registered dietitians work together to address your symptoms and find solutions that actually work for you.
Whether you’re dealing with chronic digestive issues or unpredictable symptom flare-ups, our GI specialists deliver:
✔ Personalized care plans tailored to your lifestyle
✔ Science-backed strategies to calm your gut
✔ Compassionate, whole-person care
✔ And so much more!
Ready to take control of your gut health?