New findings from Oshi Health reveal the stigma around digestive issues, which may keep millions of Americans suffering in silence rather than seeking the GI care they need.
A new national survey commissioned by Oshi Health and conducted by The Harris Poll suggests that gastrointestinal (GI) issues like bloating, reflux, constipation, and diarrhea are widespread. Yet the majority of adults ages 18-54 (52%) don’t feel very comfortable talking to a healthcare provider about their poop. That silence is costly—for the individuals suffering and beyond, at a time when healthcare costs are rising.
Here are the survey findings, plus what your provider actually wants to know about your poop (and a handy conversation guide).
Half of Americans suffer from GI issues—with many believing bloating, reflux, and more are ‘just a normal part of life’
1 in 2 Americans (50%) have either been diagnosed with a GI condition (29%) or suspect they have one, even though they don’t have a diagnosis (44%).
Yet, more than half of Americans (52%) believe digestive symptoms like abdominal pain, bloating, constipation, diarrhea, and reflux are just a normal part of life.
The majority of Americans would rather do something unpleasant than discuss their poop in a social setting
Despite widespread digestive symptoms, about 7 in 10 Americans (71%) would rather do something unpleasant than discuss their poop habits in a social setting.
- 45% would rather sit in traffic
- 35% would rather do their taxes
Men are more vocal about poop than women
The survey also found that the level of openness with which people discuss their bowel habits varies by age and gender. Men were more likely than women to feel very comfortable talking about poop in certain situations, despite IBS and other GI conditions having an outsized impact on women.
40% of men vs. 34% of women are very comfortable discussing their poop with a romantic partner.
The cost of silence is high
More people than ever are turning to the Internet first when health questions come up, often instead of seeking medical care. According to the Centers for Disease Control and Prevention (CDC), during 2022, over half of U.S. adults used the web for health-related searches. More recent data suggests that 1 in 6 adults use AI to get health information and advice—a source that can deliver unreliable, non-medically vetted answers. While online information can be helpful, it often lacks context and personalization. Some sources even lack medical oversight.
Taking it one step further, the new survey findings suggest that stigma and embarrassment around digestive symptoms and bathroom habits may drive people to search privately instead of talking to a provider.
Looking up symptoms online can be a natural starting point. But this self-directed searching can also lead to anxiety, delayed diagnoses, missed work, and cycles of costly, ineffective care—representing over $136 billion in yearly costs.
Oshi’s on a mission to show that the human and economic costs of stigma around digestive health aren’t inevitable. When people understand their symptoms and feel supported in seeking timely digestive care, they’re far more likely to find lasting relief—or even avoid a GI diagnosis altogether.
Changes in bathroom habits, for example—including blood in your stool—can sometimes be an early sign of colorectal cancer, though the disease can also develop without noticeable symptoms. That’s yet another reason to stay closely connected with a GI provider who can help you determine your risk and screening options.

It all starts with a conversation.
What your poop says about your gut health—and how to discuss it with your provider
Talking about poop can feel awkward. We get it. But your bathroom habits can tell you (and your provider) a lot about your gut health.
Why talking about poop habits matters
Changes in your stool—like how often you go, how it looks—can be early signs that something in your gut isn’t working the way it should. Bringing up these changes can help your provider spot patterns, catch problems before they get worse, and get you back to life without GI symptoms.
Poop basics
So, what does healthy poop look like? Clinicians typically use the Bristol Stool Chart to get a sense of your stool consistency. Is your poop very hard and pellet-like or loose and watery? Ideally, it should fall somewhere in between: formed yet easy to pass.
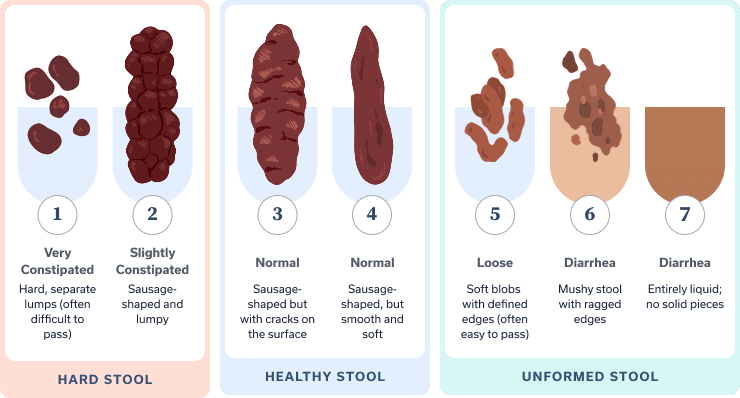
You don’t need to memorize the chart for it to be useful. Just having a general sense of where your stool usually falls on the consistency scale can help your provider. What matters most is noticing changes from your usual pattern. Surprise, surprise, poop and bathroom habits can vary a lot from person to person. Your normal is the most helpful baseline—whether that’s going three times a day to three times a week.
Here’s what your provider might ask you to get a sense of your poop patterns:
- How often are you pooping?
- What’s the consistency? (hard, loose, somewhere in between)
- Any changes in color, smell, or appearance?
- Is your poop easy or uncomfortable to pass?
- Are you ever rushing to use the bathroom?
- Any sensations of incomplete evacuation? (still feeling like you need to poop after pooping)
- Any pain, mucus, or blood?
If you notice a sudden change—more urgency, looser stools, new pain—that’s worth sharing, even if it feels like no big deal. Let your provider know when the changes started and, if you can recall, whether anything was going on at the time, like a change in diet or medication, or major stress in your life.
Tips for talking poop
First off, know that it’s almost a guarantee your provider has heard it before.
“I’ve heard and seen it all. The more detailed you are about your bowel habits, the better we are at ordering the right tests, treatments, and coming up with an accurate diagnosis,” says Oshi GI provider Gabriella McCarty.
Here are a few tips to get comfortable and effectively talk poop:
- Name your feelings. Be open about whether something feels uncomfortable for you to talk about. Your provider should understand and meet you where you are.
- Use whatever term feels right to you. Poop? Stool? Go with your preferred word choice. You might find medical terms feel less weighty. Your main job is to clearly describe your symptoms and experience.
- Write down notes before your visit. Jot down a few notes to help you remember what you want to say (e.g., I’m running to the bathroom a lot, my stool is dry and hard to pass, I’m pooping more than I used to, it started a few weeks ago).
- Ask for help describing things. Not sure how to explain something? Let your provider know! They can ask clarifying questions or offer options, like “Does it feel more like X or Y?”
Still cringing at the thought of poop talk? Practice in the mirror before your appointment. The more you say the words out loud, the less embarrassing they’ll sound to you.
Remember, this is their job! And everybody poops! Talking about poop and bathroom habits isn’t something to be embarrassed about. It’s how you get answers and a care plan for lasting relief.
This survey was conducted online within the United States by The Harris Poll on behalf of Oshi Health from January 22-26, 2026 among 2,091 adults ages 18 and older. The sampling precision of Harris online polls is measured by using a Bayesian credible interval. For this study, the sample data is accurate to within +/- 2.5 percentage points using a 95% confidence level.
About Oshi Health
Oshi Health is the only nationwide multidisciplinary gastrointestinal (GI) medical clinic combining specialized medical, dietary, and gut-brain care proven to get patients better, faster. Available to people in all 50 states with the convenience of telehealth and in-network with most insurance providers, Oshi’s care accelerates the speed to diagnosis and symptom control— significantly improving people’s quality of life.



