Many of us can recall a time when a single nerve-wracking or distressing situation has triggered an unexpected and urgent GI symptom. People suffering with chronic GI ailments live in a reality where these mental and physical triggers are multiplied, amplified and constant.
Even more notably, people living with ongoing GI symptoms may actually be more susceptible to the effects of stress than the general population. Often referred to as “high gut responders,” individuals with GI symptoms related to a history of trauma and chronic stress become hypervigilant and hypersensitive to the 24/7 communication between the brain and gut.
Too often, people seeking GI symptom relief pursue medical solutions and remedies, although medical doctors don’t always understand the very real — and very treatable — psychological phenomenon. Even GI specialists and general mental health practitioners may not be aware of the intricacies of the mind-gut connection as related to GI conditions, let alone know how to implement the clinically powerful tools to address it.
The scientific evidence shows that GI-specialized psychological interventions are some of the most clinically effective in the field of psychology — capable of driving significant control over GI symptoms with sustainable and life-changing impact.
Digestive and emotional health are undoubtedly interconnected, and anatomically proven. Shouldn’t treatments for GI symptoms regularly incorporate psychological and behavioral interventions?
The reality of mind-gut anatomy
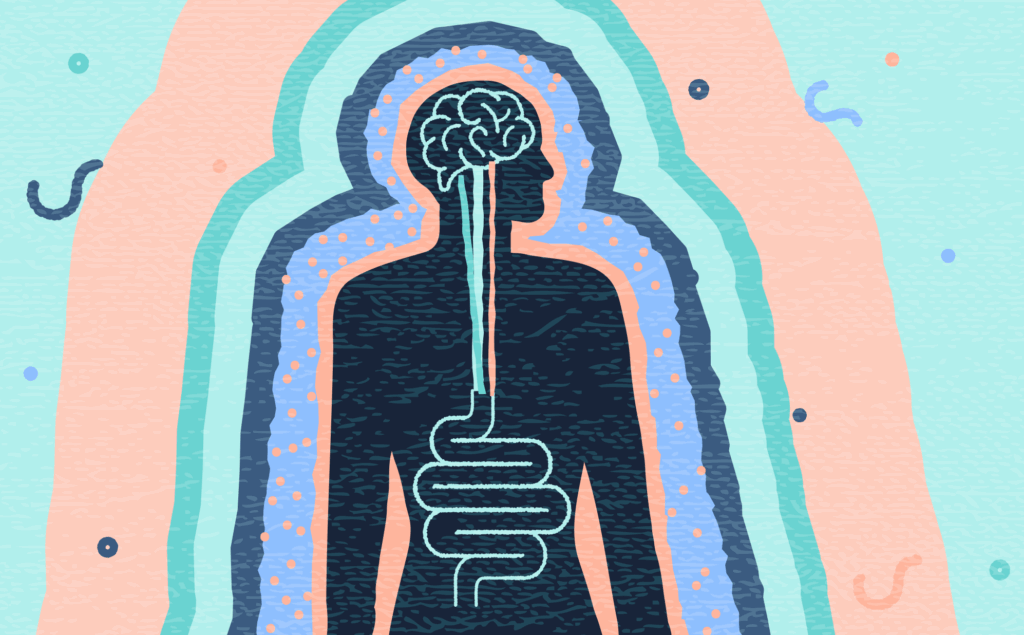
You’ve heard about the “brain-gut connection,” or the notion that “the gut is the second brain” – but did you know the phrases stem from our anatomy and physiology?
Let’s start with some biochemistry as proof of the interconnectedness of mind and gut: Bacteria in the gut produce more than 95% of the body’s supply of serotonin and 50% of the dopamine, which are two of the main factors regulating mood, sleep and digestion.
Physiologically, the brain-gut anatomy that impacts communication includes the enteric, sympathetic and parasympathetic nervous systems. Indeed, the digestive system has the largest accumulation of neurons outside the brain. The vagus nerve is the key connection between the nerve cells and the brain. The longest cranial nerve in the body, the vagus nerve serves as the 2-way neural communication conduit between the brain and the digestive organs. It regulates muscle contraction, and controls gut sensations and gland secretions in the digestive system.
The vagus nerve is also a key instrument in the parasympathetic nervous system, which oversees critical body functions like digestion, heart and respiration rates, immune system, inflammation modulation and mood response.
In people with chronic GI issues, the brain can over-amplify pain signals like urgency, nausea, bloating and GI discomfort, which means that their sympathetic nervous system is in a dysregulated state, and normal communication is disrupted.
The most incredible part of brain-gut psychology? By taking control of a core human process — respiration; yes, breathing — a person can actually harness the vagus nerve, and engage the parasympathetic nervous system in order to regulate digestion. This happens because the vagus nerve passes through the diaphragm. Diaphragmatic breathing (youtube.com/watch?v=ub3tsaiebny) works because it stimulates the vagus nerve, which turns on the parasympathetic nervous system, which regulates digestion.
In other words: Specialized practices of activating mindful respiration like breathing exercises, meditation and yoga, can take a person out of a chronic dysregulated digestive state.
Disrupt mind-gut signals; control GI symptoms
Using an entirely different mechanism than physiological interventions, GI psychology uses tools and resources to influence the brain-gut connection. These treatments alter the dysregulated signals between the brain and the GI tract, encourage new neural pathways, increase resilience, reduce the severity and occurrence of symptoms, and improve quality of life.
These mindfulness and cognitive behavioral treatments and coping strategies are backed by more than 30 years of research, and are executed by psychologists who are specially trained in treating the mental and behavioral aspects of GI conditions.
Having already mentioned diaphragmatic breathing, here’s a look at several additional tools that GI psychologists use with their patients, and some of the key aspects of each:
Cognitive behavioral therapy (CBT)
• Collaborative approach to help people learn new coping skills, change their thought process, examine the evidence at the source of anxiety to reframe their perspective
• New ways of thinking and behaving to reduce stress and uncomfortable symptoms (e.g. diaphragmatic breathing)
• Encouraging people to practice and do “homework” outside of sessions (e.g. journaling, recording thoughts and using specific strategies to restructure beliefs.)
Gut-directed hypnotherapy
• Deep form of relaxation, guided imagery, verbal suggestions
• Gut-brain communication is more receptive to helpful suggestion in this state
Acceptance and commitment therapy
• Learn to accept and live with diagnosis, symptoms, and stop catastrophizing
• To manage GI symptoms, instead of avoiding life due to discomfort or concern, engage in activities that serve personal values and enrich life’s experience
Motivational interviewing (MI)
• Because individuals with GI conditions are often asked to make so many changes for their health, MI is a proven approach to guide health behavior change through enhanced motivation, confidence and commitment
Other useful tools include; Psychodynamic Interpersonal Therapy, Solutions-Focused Brief Therapy and Mindful-based Stress Reduction.
Breaking the vicious cycle
For many people suffering with chronic GI ailments, the unpredictable, uncontrolled and uncomfortable symptoms are pervasive, and can be traumatizing.
The cycle of distress goes like this: Experiencing unpleasant GI symptoms leads people to hyper-focus on the potential of an embarrassing or painful recurrence – also called catastrophizing. This triggers fear and anxiety, which disrupts the normal mind-gut communication system. The resulting cognitive distortion can actually aggravate or trigger a new onset of GI symptoms.
Secondary to this cycle, people may also develop negative, fearful or unhealthy relationships or associations with food and the very experience of eating.
This disproportionate fear and anxiety around food and GI symptoms leads people to miss work, avoid social engagements and food-related events, and outings of any kind. Predictably, this “shrinking” of the key elements of daily happiness has a detrimental impact on their quality of life, causing isolation, anxiety and depression.
Effective, empowering, life-changing
Psychological and behavioral health interventions for GI symptoms are life-changing and impactful, yielding rapid and sustained symptom control, often within 5 sessions. With regular practice, the treatment is durable and ongoing, lasting years.
With a heavy focus on patient-driven daily practices at home, this treatment empowers people with the tools to take control and affect change themselves. People regain confidence and control, and are truly vested and involved in their own treatment and outcomes. This proactive – versus reactive – position is a significant and gratifying power shift for people who have changed their entire lives to accommodate their GI illness.
Additionally, knowing that their chronic GI and associated mental health issues are not “all in their head” is incredibly validating. The mystery of unpredictability is gone, once people recognize that they can take some control of symptoms on their own.
People can fully re-engage with life, work, family and friends. Since their GI symptoms are largely controlled, there is no escalation to costly ER visits or invasive procedures. There are virtually no known side effects. In fact, behavioral GI treatments are often so effective at decreasing symptoms, there is less need for medication.
It results in a complete re-framing of living with chronic GI illness, with positive impacts on productivity, health economics, and quality of life.
Oshi is your partner in digestive health
Feel like your digestive concerns are running your life? You’re not alone—and we’re here to help you find lasting relief.
Oshi Health GI providers, gut-brain specialists, and registered dietitians work together to address your symptoms and find solutions that actually work for you.
Whether you’re dealing with chronic digestive issues or unpredictable symptom flare-ups, our GI specialists deliver:
✔ Personalized care plans tailored to your lifestyle
✔ Science-backed strategies to calm your gut
✔ Compassionate, whole-person care
✔ And so much more!
Ready to take control of your gut health?